
- Current
- Browse
- Collections
-
For contributors
- For Authors
- Instructions to authors
- Article processing charge
- e-submission
- For Reviewers
- Instructions for reviewers
- How to become a reviewer
- Best reviewers
- For Readers
- Readership
- Subscription
- Permission guidelines
- About
- Editorial policy
Search
- Page Path
- HOME > Search
- Guideline/Fact Sheet
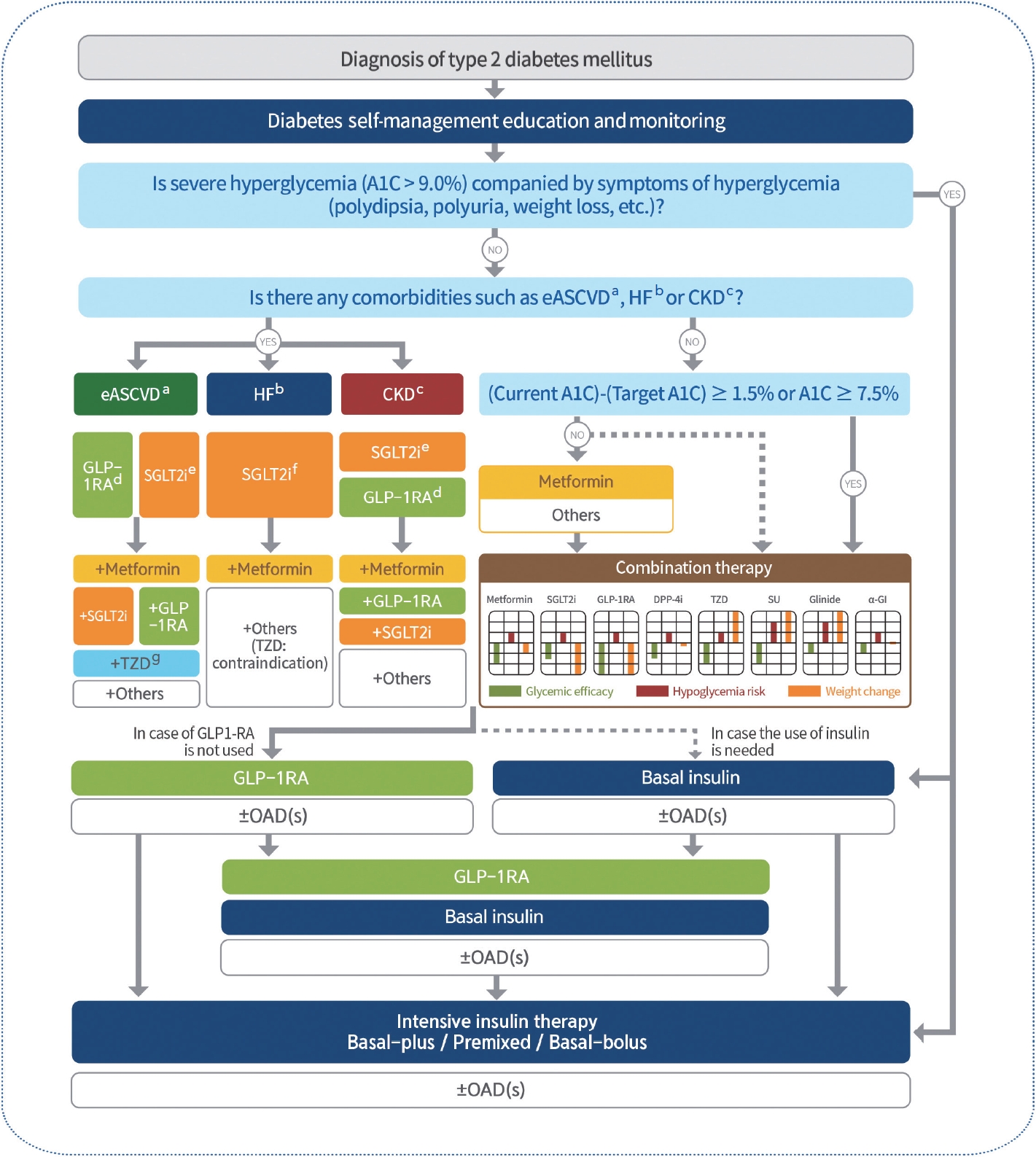
- 2023 Clinical Practice Guidelines for Diabetes Mellitus of the Korean Diabetes Association
- Jong Han Choi, Kyung Ae Lee, Joon Ho Moon, Suk Chon, Dae Jung Kim, Hyun Jin Kim, Nan Hee Kim, Ji A Seo, Mee Kyoung Kim, Jeong Hyun Lim, YoonJu Song, Ye Seul Yang, Jae Hyeon Kim, You-Bin Lee, Junghyun Noh, Kyu Yeon Hur, Jong Suk Park, Sang Youl Rhee, Hae Jin Kim, Hyun Min Kim, Jung Hae Ko, Nam Hoon Kim, Chong Hwa Kim, Jeeyun Ahn, Tae Jung Oh, Soo-Kyung Kim, Jaehyun Kim, Eugene Han, Sang-Man Jin, Won Suk Choi, Min Kyong Moon, Committee of Clinical Practice Guidelines, Korean Diabetes Association
- Diabetes Metab J. 2023;47(5):575-594. Published online September 26, 2023
- DOI: https://doi.org/10.4093/dmj.2023.0282
- 5,231 View
- 645 Download
- 8 Web of Science
- 15 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - In May 2023, the Committee of Clinical Practice Guidelines of the Korean Diabetes Association published the revised clinical practice guidelines for Korean adults with diabetes and prediabetes. We incorporated the latest clinical research findings through a comprehensive systematic literature review and applied them in a manner suitable for the Korean population. These guidelines are designed for all healthcare providers nationwide, including physicians, diabetes experts, and certified diabetes educators who manage patients with diabetes or individuals at risk of developing diabetes. Based on recent changes in international guidelines and the results of a Korean epidemiological study, the recommended age for diabetes screening has been lowered. In collaboration with the relevant Korean medical societies, recently revised guidelines for managing hypertension and dyslipidemia in patients with diabetes have been incorporated into this guideline. An abridgment containing practical information on patient education and systematic management in the clinic was published separately.
-
Citations
Citations to this article as recorded by- Mortality in metabolic dysfunction-associated steatotic liver disease: A nationwide population-based cohort study
Eugene Han, Byung-Wan Lee, Eun Seok Kang, Bong-Soo Cha, Sang Hoon Ahn, Yong-ho Lee, Seung Up Kim
Metabolism.2024; 152: 155789. CrossRef - Letter by In-Kyung Jeong Regarding Article, Trends in Prevalence of Hypertriglyceridemia and Related Factors in Korean Adults: A Serial Cross-Sectional Study
In-Kyung Jeong
Journal of Lipid and Atherosclerosis.2024; 13(1): 80. CrossRef - Association between cardiovascular disease risk and incident type 2 diabetes mellitus in individuals with prediabetes: A retrospective cohort study
Myung Jin Kim, Yun Kyung Cho, Chang Hee Jung, Woo Je Lee
Diabetes Research and Clinical Practice.2024; 208: 111125. CrossRef - Korea Hypertension Fact Sheet 2023: analysis of nationwide population-based data with a particular focus on hypertension in special populations
Hyeon Chang Kim, Hokyou Lee, Hyeok-Hee Lee, Dasom Son, Minsung Cho, Sojung Shin, Yeeun Seo, Eun-Jin kim, Song Vogue Ahn, Sun Ha Jee, Sungha Park, Hae-Young Lee, Min Ho Shin, Sang-Hyun Ihm, Seung Won Lee, Jong Ku Park, Il Suh, Tae-Yong Lee
Clinical Hypertension.2024;[Epub] CrossRef - Diabetes Duration, Cholesterol Levels, and Risk of Cardiovascular Diseases in Individuals With Type 2 Diabetes
Mee Kyoung Kim, Kyu Na Lee, Kyungdo Han, Seung-Hwan Lee
The Journal of Clinical Endocrinology & Metabolism.2024;[Epub] CrossRef - Effect of Adding Apolipoprotein B Testing on the Prevalence of Dyslipidemia and Risk of Cardiovascular Disease in the Korean Adult Population
Rihwa Choi, Sang Gon Lee, Eun Hee Lee
Metabolites.2024; 14(3): 169. CrossRef - A self-powered and supercapacitive microneedle continuous glucose monitoring system with a wide range of glucose detection capabilities
Hye-Jun Kil, Jang Hyeon Kim, Kanghae Lee, Tae-Uk Kang, Ju-Hyun Yoo, Yong-ho Lee, Jin-Woo Park
Biosensors and Bioelectronics.2024; 257: 116297. CrossRef - Cardiorenal outcomes and mortality after sodium‐glucose cotransporter‐2 inhibitor initiation in type 2 diabetes patients with percutaneous coronary intervention history
Jin Hwa Kim, Young Sang Lyu, BongSeong Kim, Mee Kyung Kim, Sang Yong Kim, Ki‐Hyun Baek, Ki‐Ho Song, Kyungdo Han, Hyuk‐Sang Kwon
Diabetes, Obesity and Metabolism.2024;[Epub] CrossRef - SGLT2i impact on HCC incidence in patients with fatty liver disease and diabetes: a nation-wide cohort study in South Korea
Hyo Jung Cho, Eunyoung Lee, Soon Sun Kim, Jae Youn Cheong
Scientific Reports.2024;[Epub] CrossRef - Management of Dyslipidemia in Patients with Diabetes Mellitus
Kyung Ae Lee
The Journal of Korean Diabetes.2023; 24(3): 111. CrossRef - 2023 Clinical Practice Guidelines for Diabetes: Recommendations for Pharmacological Treatment of Type 2 Diabetes
Junghyun Noh
The Journal of Korean Diabetes.2023; 24(3): 127. CrossRef - 2023 Clinical Practice Guidelines for Diabetes
Min Kyong Moon
The Journal of Korean Diabetes.2023; 24(3): 120. CrossRef - 2023 Clinical Practice Guidelines for Diabetes: Management of Cardiovascular Risk Factors
Ye Seul Yang
The Journal of Korean Diabetes.2023; 24(3): 135. CrossRef - A 33-Year-Old Man Presented with Abdominal Pain and Vomiting Starting a Day Ago
Jong Han Choi
The Korean Journal of Medicine.2023; 98(6): 289. CrossRef - Comorbidity Patterns and Management in Inpatients with Endocrine Diseases by Age Groups in South Korea: Nationwide Data
Sung-Soo Kim, Hun-Sung Kim
Journal of Personalized Medicine.2023; 14(1): 42. CrossRef
- Mortality in metabolic dysfunction-associated steatotic liver disease: A nationwide population-based cohort study
- Drug/Regimen
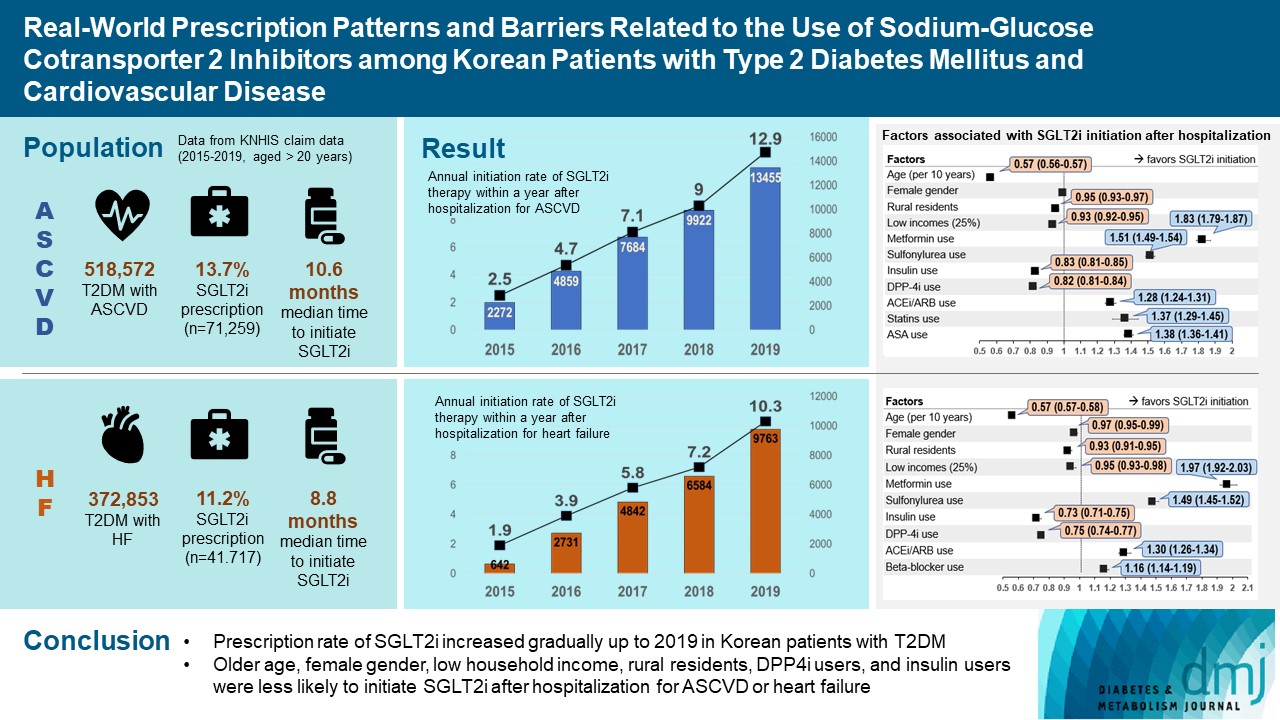
- Real-World Prescription Patterns and Barriers Related to the Use of Sodium-Glucose Cotransporter 2 Inhibitors among Korean Patients with Type 2 Diabetes Mellitus and Cardiovascular Disease
- Jong Ha Baek, Ye Seul Yang, Seung-Hyun Ko, Kyung Do Han, Jae Hyeon Kim, Min Kyong Moon, Jong Suk Park, Byung-Wan Lee, Tae Jung Oh, Suk Chon, Jong Han Choi, Kyu Yeon Hur, Committee of Clinical Practice Guidelines, Korean Diabetes Association
- Diabetes Metab J. 2022;46(5):701-712. Published online June 3, 2022
- DOI: https://doi.org/10.4093/dmj.2022.0002
- 4,987 View
- 319 Download
- 6 Web of Science
- 8 Crossref
-
 Graphical Abstract
Graphical Abstract
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub 
- Background
To evaluate prescription trends and clinical factors of the sodium-glucose cotransporter 2 inhibitors (SGLT2i) use according to the presence of atherosclerotic cardiovascular disease (ASCVD) or heart failure (HF) in Korean patients with type 2 diabetes mellitus (T2DM).
Methods
Prescription patterns of SGLT2i use between 2015 and 2019 were determined using the Korean National Health Insurance Service database of claims.
Results
Of all patients with T2DM (n=4,736,493), the annual prescription rate of SGLT2i increased every year in patients with ASCVD (from 2.2% to 10.7%) or HF (from 2.0% to 11.1%). After the first hospitalization for ASCVD (n=518,572), 13.7% (n=71,259) of patients initiated SGLT2i with a median of 10.6 months. After hospitalization for HF (n=372,853), 11.2% (n=41,717) of patients initiated SGLT2i after a median of 8.8 months. In multivariate regression for hospitalization, older age (per 10 years, odds ratio [OR], 0.57; 95% confidence interval [CI], 0.56 to 0.57), lower household income (OR, 0.93; 95% CI, 0.92 to 0.95), rural residents (OR, 0.95; 95% CI, 0.93 to 0.97), and dipeptidyl peptidase-4 inhibitor (DPP-4i) users (OR, 0.82; 95% CI, 0.81 to 0.84) were associated with lesser initiation of SGLT2i in ASCVD. Additionally, female gender (OR, 0.97; 95% CI, 0.95 to 0.99) was associated with lesser initiation of SGLT2i in HF.
Conclusion
The prescription rate of SGLT2i increased gradually up to 2019 but was suboptimal in patients with ASCVD or HF. After the first hospitalization for ASCVD or HF, older age, female gender, low household income, rural residents, and DPP-4i users were less likely to initiate SGLT2i. -
Citations
Citations to this article as recorded by- Effectiveness and safety of sodium–glucose cotransporter 2 inhibitors in Asian populations
Kyoung Hwa Ha, Dae Jung Kim
Journal of Diabetes Investigation.2024; 15(3): 285. CrossRef - Real-World Treatment Patterns according to Clinical Practice Guidelines in Patients with Type 2 Diabetes Mellitus and Established Cardiovascular Disease in Korea: Multicenter, Retrospective, Observational Study
Ye Seul Yang, Nam Hoon Kim, Jong Ha Baek, Seung-Hyun Ko, Jang Won Son, Seung-Hwan Lee, Sang Youl Rhee, Soo-Kyung Kim, Tae Seo Sohn, Ji Eun Jun, In-Kyung Jeong, Chong Hwa Kim, Keeho Song, Eun-Jung Rhee, Junghyun Noh, Kyu Yeon Hur
Diabetes & Metabolism Journal.2024; 48(2): 279. CrossRef - Hospital Readmissions for Fluid Overload among Individuals with Diabetes and Diabetic Kidney Disease: Risk Factors and Multivariable Prediction Models
Jiashen Cai, Dorothy Huang, Hanis Binte Abdul Kadir, Zhihua Huang, Li Choo Ng, Andrew Ang, Ngiap Chuan Tan, Yong Mong Bee, Wei Yi Tay, Chieh Suai Tan, Cynthia C. Lim
Nephron.2024; : 1. CrossRef - Prescribing patterns of SGLT-2 inhibitors for patients with heart failure: A two-center analysis
Teja Chakrala, Roshni O. Prakash, Justin Kim, Hanzhi Gao, Umar Ghaffar, Jaymin Patel, Alex Parker, Bhagwan Dass
American Heart Journal Plus: Cardiology Research and Practice.2023; 28: 100286. CrossRef - Risk of developing chronic kidney disease in young-onset Type 2 diabetes in Korea
Joonyub Lee, Seung-Hwan Lee, Kun-Ho Yoon, Jae Hyoung Cho, Kyungdo Han, Yeoree Yang
Scientific Reports.2023;[Epub] CrossRef - Comparison of SGLT2 inhibitors with DPP-4 inhibitors combined with metformin in patients with acute myocardial infarction and diabetes mellitus
Young Sang Lyu, Seok Oh, Jin Hwa Kim, Sang Yong Kim, Myung Ho Jeong
Cardiovascular Diabetology.2023;[Epub] CrossRef - Severe hypoglycemia as a risk factor for cardiovascular outcomes in patients with type 2 diabetes: is it preventable?
Seung-Hyun Ko
Cardiovascular Prevention and Pharmacotherapy.2022; 4(3): 106. CrossRef - Association between the Diabetes Drug Cost and Cardiovascular Events and Death in Korea: A National Health Insurance Service Database Analysis
Seung Min Chung, Ji-In Lee, Eugene Han, Hyun-Ae Seo, Eonju Jeon, Hye Soon Kim, Ji Sung Yoon
Endocrinology and Metabolism.2022; 37(5): 759. CrossRef
- Effectiveness and safety of sodium–glucose cotransporter 2 inhibitors in Asian populations
- Guideline/Fact Sheet
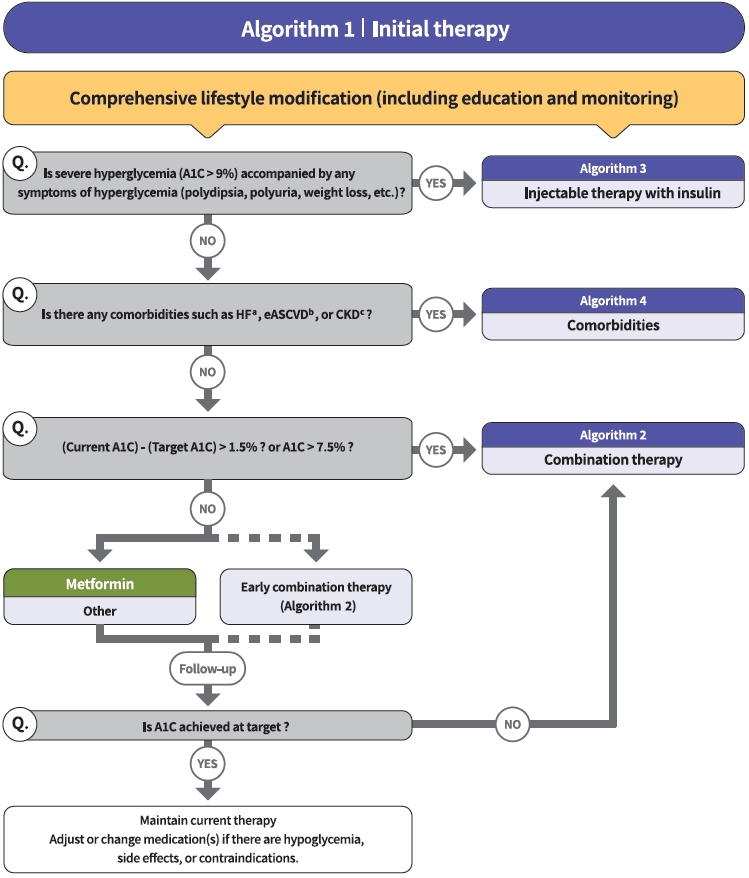
- 2021 Clinical Practice Guidelines for Diabetes Mellitus in Korea
- Kyu Yeon Hur, Min Kyong Moon, Jong Suk Park, Soo-Kyung Kim, Seung-Hwan Lee, Jae-Seung Yun, Jong Ha Baek, Junghyun Noh, Byung-Wan Lee, Tae Jung Oh, Suk Chon, Ye Seul Yang, Jang Won Son, Jong Han Choi, Kee Ho Song, Nam Hoon Kim, Sang Yong Kim, Jin Wha Kim, Sang Youl Rhee, You-Bin Lee, Sang-Man Jin, Jae Hyeon Kim, Chong Hwa Kim, Dae Jung Kim, SungWan Chun, Eun-Jung Rhee, Hyun Min Kim, Hyun Jung Kim, Donghyun Jee, Jae Hyun Kim, Won Seok Choi, Eun-Young Lee, Kun-Ho Yoon, Seung-Hyun Ko, Committee of Clinical Practice Guidelines, Korean Diabetes Association
- Diabetes Metab J. 2021;45(4):461-481. Published online July 30, 2021
- DOI: https://doi.org/10.4093/dmj.2021.0156
- 24,136 View
- 1,634 Download
- 122 Web of Science
- 141 Crossref
-
 Graphical Abstract
Graphical Abstract
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub 
- The Committee of Clinical Practice Guidelines of the Korean Diabetes Association (KDA) updated the previous clinical practice guidelines for Korean adults with diabetes and prediabetes and published the seventh edition in May 2021. We performed a comprehensive systematic review of recent clinical trials and evidence that could be applicable in real-world practice and suitable for the Korean population. The guideline is provided for all healthcare providers including physicians, diabetes experts, and certified diabetes educators across the country who manage patients with diabetes or the individuals at the risk of developing diabetes mellitus. The recommendations for screening diabetes and glucose-lowering agents have been revised and updated. New sections for continuous glucose monitoring, insulin pump use, and non-alcoholic fatty liver disease in patients with diabetes mellitus have been added. The KDA recommends active vaccination for coronavirus disease 2019 in patients with diabetes during the pandemic. An abridgement that contains practical information for patient education and systematic management in the clinic was published separately.
-
Citations
Citations to this article as recorded by- Impact of Subclinical Atrial Function on the Prognosis of Patients With Atrial Fibrillation and Metabolic Syndrome
Hyun-Jin Kim
CardioMetabolic Syndrome Journal.2024; 4(1): 36. CrossRef - Associations of omega-3 fatty acids vs. fenofibrate with adverse cardiovascular outcomes in people with metabolic syndrome: propensity matched cohort study
Nam Hoon Kim, Ji Yoon Kim, Jimi Choi, Sin Gon Kim
European Heart Journal - Cardiovascular Pharmacotherapy.2024; 10(2): 118. CrossRef - A Multicenter, Randomized, Open-Label Study to Compare the Effects of Gemigliptin Add-on or Escalation of Metformin Dose on Glycemic Control and Safety in Patients with Inadequately Controlled Type 2 Diabetes Mellitus Treated with Metformin and SGLT-2 Inh
Hae Jin Kim, Jung Hyun Noh, Min Kyong Moon, Sung Hee Choi, Seung-Hyun Ko, Eun-Jung Rhee, Kyu Yeon Hur, In-Kyung Jeong, Mark Yorek
Journal of Diabetes Research.2024; 2024: 1. CrossRef - Efficacy and Safety of Once-Weekly Semaglutide Versus Once-Daily Sitagliptin as Metformin Add-on in a Korean Population with Type 2 Diabetes
Byung-Wan Lee, Young Min Cho, Sin Gon Kim, Seung-Hyun Ko, Soo Lim, Amine Dahaoui, Jin Sook Jeong, Hyo Jin Lim, Jae Myung Yu
Diabetes Therapy.2024; 15(2): 547. CrossRef - Real-World Continuous Glucose Monitoring Data from a Population with Type 1 Diabetes in South Korea: Nationwide Single-System Analysis
Ji Yoon Kim, Sang-Man Jin, Sarah B. Andrade, Boyang Chen, Jae Hyeon Kim
Diabetes Technology & Therapeutics.2024;[Epub] CrossRef - Association between Dyslipidemia and Glycated Hemoglobin in a Population-Based Study
Purum Kang, Ka Young Kim, Hye Young Shin
Metabolites.2024; 14(2): 92. CrossRef - Outcomes of Various Classes of Oral Antidiabetic Drugs on Nonalcoholic Fatty Liver Disease
Heejoon Jang, Yeonjin Kim, Dong Hyeon Lee, Sae Kyung Joo, Bo Kyung Koo, Soo Lim, Woojoo Lee, Won Kim
JAMA Internal Medicine.2024; 184(4): 375. CrossRef - View on Metformin: Antidiabetic and Pleiotropic Effects, Pharmacokinetics, Side Effects, and Sex-Related Differences
Guglielmina Froldi
Pharmaceuticals.2024; 17(4): 478. CrossRef - Comparison between a tubeless, on-body automated insulin delivery system and a tubeless, on-body sensor-augmented pump in type 1 diabetes: a multicentre randomised controlled trial
Ji Yoon Kim, Sang-Man Jin, Eun Seok Kang, Soo Heon Kwak, Yeoree Yang, Jee Hee Yoo, Jae Hyun Bae, Jun Sung Moon, Chang Hee Jung, Ji Cheol Bae, Sunghwan Suh, Sun Joon Moon, Sun Ok Song, Suk Chon, Jae Hyeon Kim
Diabetologia.2024;[Epub] CrossRef - Inhibition of sodium-glucose cotransporter-2 and liver-related complications in individuals with diabetes: a Mendelian randomization and population-based cohort study
Sung Won Chung, Hye-Sung Moon, Hyunjae Shin, Hyein Han, Sehoon Park, Heejin Cho, Jeayeon Park, Moon Haeng Hur, Min Kyung Park, Sung-Ho Won, Yun Bin Lee, Eun Ju Cho, Su Jong Yu, Dong Ki Kim, Jung-Hwan Yoon, Jeong-Hoon Lee, Yoon Jun Kim
Hepatology.2024;[Epub] CrossRef - Efficacy of intermittent short‐term use of a real‐time continuous glucose monitoring system in non‐insulin–treated patients with type 2 diabetes: A randomized controlled trial
Sun Joon Moon, Kyung‐Soo Kim, Woo Je Lee, Mi Yeon Lee, Robert Vigersky, Cheol‐Young Park
Diabetes, Obesity and Metabolism.2023; 25(1): 110. CrossRef - Therapeutic Effects of Switching to Anagliptin from Other DPP-4 Inhibitors in T2DM Patients with Inadequate Glycemic Control: A Non-interventional, Single-Arm, Open-Label, Multicenter Observational Study
Sang-Yong Kim, Sungrae Kim
Diabetes Therapy.2023; 14(1): 109. CrossRef - Low Skeletal Muscle Mass Accompanied by Abdominal Obesity Additively Increases the Risk of Incident Type 2 Diabetes
Ji Eun Jun, Seung-Eun Lee, You-Bin Lee, Gyuri Kim, Sang-Man Jin, Jae Hwan Jee, Jae Hyeon Kim
The Journal of Clinical Endocrinology & Metabolism.2023; 108(5): 1173. CrossRef - Diabetes screening in South Korea: a new estimate of the number needed to screen to detect diabetes
Kyoung Hwa Ha, Kyung Ae Lee, Kyung-Do Han, Min Kyong Moon, Dae Jung Kim
The Korean Journal of Internal Medicine.2023; 38(1): 93. CrossRef - Justicia carnea extracts ameliorated hepatocellular damage in streptozotocin-induced type 1 diabetic male rats via decrease in oxidative stress, inflammation and increasing other risk markers
John Adeolu Falode, Oluwaseun Igbekele Ajayi, Tolulope Victoria Isinkaye, Akinwunmi Oluwaseun Adeoye, Basiru Olaitan Ajiboye, Bartholomew I. C. Brai
Biomarkers.2023; 28(2): 177. CrossRef - Sex differences in the impact of diabetes mellitus on tuberculosis recurrence: a retrospective national cohort study
Dararat Eksombatchai, Dawoon Jeong, Jeongha Mok, Doosoo Jeon, Hee-Yeon Kang, Hee Jin Kim, Hee-Sun Kim, Hongjo Choi, Young Ae Kang
International Journal of Infectious Diseases.2023; 127: 1. CrossRef - The Predictive Ability of C-Peptide in Distinguishing Type 1 Diabetes From Type 2 Diabetes: A Systematic Review and Meta-Analysis
Sajid Iqbal, Abdulrahim Abu Jayyab, Ayah Mohammad Alrashdi, Silvia Reverté-Villarroya
Endocrine Practice.2023; 29(5): 379. CrossRef - Anagliptin twice‐daily regimen improves glycaemic variability in subjects with type 2 diabetes: A double‐blind, randomized controlled trial
Yong‐ho Lee, Doo‐Man Kim, Jae Myung Yu, Kyung Mook Choi, Sin Gon Kim, Kang Seo Park, Hyun‐Shik Son, Choon Hee Chung, Kyu Jeung Ahn, Soon Hee Lee, Ki‐Ho Song, Su Kyoung Kwon, Hyeong Kyu Park, Kyu Chang Won, Hak Chul Jang
Diabetes, Obesity and Metabolism.2023; 25(5): 1174. CrossRef - Implementation of five machine learning methods to predict the 52-week blood glucose level in patients with type 2 diabetes
Xiaomin Fu, Yuhan Wang, Ryan S. Cates, Nan Li, Jing Liu, Dianshan Ke, Jinghua Liu, Hongzhou Liu, Shuangtong Yan
Frontiers in Endocrinology.2023;[Epub] CrossRef - Lipid Management in Korean People With Type 2 Diabetes Mellitus: Korean Diabetes Association and Korean Society of Lipid and Atherosclerosis Consensus Statement
Ye Seul Yang, Hack-Lyoung Kim, Sang-Hyun Kim, Min Kyong Moon
Journal of Lipid and Atherosclerosis.2023; 12(1): 12. CrossRef - The Efficacy of Treatment Intensification by Quadruple Oral Therapy Compared to GLP-1RA Therapy in Poorly Controlled Type 2 Diabetes Mellitus Patients: A Real-world Data Study
Minyoung Kim, Hosu Kim, Kyong Young Kim, Soo Kyoung Kim, Junghwa Jung, Jong Ryeal Hahm, Jaehoon Jung, Jong Ha Baek
Diabetes & Metabolism Journal.2023; 47(1): 135. CrossRef - Safety and Effectiveness of Empagliflozin in Korean Patients with Type 2 Diabetes Mellitus: Results from a Nationwide Post-Marketing Surveillance
Jun Sung Moon, Nam Hoon Kim, Jin Oh Na, Jae Hyoung Cho, In-Kyung Jeong, Soon Hee Lee, Ji-Oh Mok, Nan Hee Kim, Dong Jin Chung, Jinhong Cho, Dong Woo Lee, Sun Woo Lee, Kyu Chang Won
Diabetes & Metabolism Journal.2023; 47(1): 82. CrossRef - Evaluation and Management of Patients With Diabetes and Heart Failure: A Korean Diabetes Association and Korean Society of Heart Failure Consensus Statement
Kyu-Sun Lee, Junghyun Noh, Seong-Mi Park, Kyung Mook Choi, Seok-Min Kang, Kyu-Chang Won, Hyun-Jai Cho, Min Kyong Moon
International Journal of Heart Failure.2023; 5(1): 1. CrossRef - Influenza vaccination trend and related factors among patients with diabetes in Korea: Analysis using a nationwide database
Dong-Hwa Lee, Bumhee Yang, Seonhye Gu, Eung-Gook Kim, Youlim Kim, Hyung Koo Kang, Yeong Hun Choe, Hyun Jeong Jeon, Seungyong Park, Hyun Lee
Frontiers in Endocrinology.2023;[Epub] CrossRef - Optimal Low-Density Lipoprotein Cholesterol Level for Primary Prevention in Koreans with Type 2 Diabetes Mellitus
Ji Yoon Kim, Nam Hoon Kim
Diabetes & Metabolism Journal.2023; 47(1): 42. CrossRef - Evaluation and Management of Patients with Diabetes and Heart Failure: A Korean Diabetes Association and Korean Society of Heart Failure Consensus Statement
Kyu-Sun Lee, Junghyun Noh, Seong-Mi Park, Kyung Mook Choi, Seok-Min Kang, Kyu-Chang Won, Hyun-Jai Cho, Min Kyong Moon
Diabetes & Metabolism Journal.2023; 47(1): 10. CrossRef - Lipid Management in Korean People with Type 2 Diabetes Mellitus: Korean Diabetes Association and Korean Society of Lipid and Atherosclerosis Consensus Statement
Ye Seul Yang, Hack-Lyoung Kim, Sang-Hyun Kim, Min Kyong Moon
Diabetes & Metabolism Journal.2023; 47(1): 1. CrossRef - Association between Low-Density Lipoprotein Cholesterol Level and Cardiovascular Outcomes in Korean Adults: A Nationwide Cohort Study
Junghyun Noh, Min Kyong Moon, Eun-Jung Rhee, Sang Hyun Park, Hyeon Chang Kim, Byung Jin Kim, Hae Jin Kim, Seonghoon Choi, Jin Oh Na, Young Youl Hyun, Bum Joon Kim, Kyung-Do Han, In-Kyung Jeong
Diabetes & Metabolism Journal.2023; 47(1): 59. CrossRef - Analysis of the Incidence of Type 2 Diabetes, Requirement of Insulin Treatment, and Diabetes-Related Complications among Patients with Cancer
Su Jung Lee, Chulho Kim, Hyunjae Yu, Dong-Kyu Kim
Cancers.2023; 15(4): 1094. CrossRef - The 2022 focused update of the 2018 Korean Hypertension Society Guidelines for the management of hypertension
Hack-Lyoung Kim, Eun Mi Lee, Shin Young Ahn, Kwang-il Kim, Hyeon Chang Kim, Ju Han Kim, Hae-Young Lee, Jang Hoon Lee, Jong-Moo Park, Eun Joo Cho, Sungha Park, Jinho Shin, Young-Kwon Kim
Clinical Hypertension.2023;[Epub] CrossRef - Consistency of 1-day and 3-day average dietary intake and the relationship of dietary intake with blood glucose, hbA1c, BMI, and lipids in patients with type 2 diabetes
DaeEun Lee, Haejung Lee, Sangeun Lee, MinJin Lee, Ah Reum Khang
Journal of Korean Biological Nursing Science.2023; 25(1): 20. CrossRef - Efficacy and safety of enavogliflozin versus dapagliflozin added to metformin plus gemigliptin treatment in patients with type 2 diabetes: A double-blind, randomized, comparator-active study: ENHANCE-D study
Kyung-Soo Kim, Kyung Ah Han, Tae Nyun Kim, Cheol-Young Park, Jung Hwan Park, Sang Yong Kim, Yong Hyun Kim, Kee Ho Song, Eun Seok Kang, Chul Sik Kim, Gwanpyo Koh, Jun Goo Kang, Mi Kyung Kim, Ji Min Han, Nan Hee Kim, Ji Oh Mok, Jae Hyuk Lee, Soo Lim, Sang S
Diabetes & Metabolism.2023; 49(4): 101440. CrossRef - Effect of olmesartan and amlodipine on serum angiotensin-(1–7) levels and kidney and vascular function in patients with type 2 diabetes and hypertension
Kyuho Kim, Ji Hye Moon, Chang Ho Ahn, Soo Lim
Diabetology & Metabolic Syndrome.2023;[Epub] CrossRef - Menopausal hormone therapy and the risk of type 2 diabetes mellitus: Health Insurance Database in South Korea–based retrospective cohort study
Jin-Sung Yuk, Jung Min Kim
Menopause.2023; 30(5): 497. CrossRef - Intensified Multifactorial Intervention in Patients with Type 2 Diabetes Mellitus
Takayoshi Sasako, Toshimasa Yamauchi, Kohjiro Ueki
Diabetes & Metabolism Journal.2023; 47(2): 185. CrossRef - Association between antidiabetic drugs and the incidence of atrial fibrillation in patients with type 2 diabetes: A nationwide cohort study in South Korea
Sunyoung Kim, So Young Park, Bongseong Kim, Chanyang Min, Wonyoung Cho, Dong Keon Yon, Joo Young Kim, Kyung-Do Han, Eun-Jung Rhee, Won-Young Lee, Sang Youl Rhee
Diabetes Research and Clinical Practice.2023; 198: 110626. CrossRef - Totally robotic Roux-en-Y gastric bypass in a morbidly obese patient in Korea: a case report
Ji Won Seo, Kyong-Hwa Jun
Journal of Minimally Invasive Surgery.2023; 26(1): 40. CrossRef - Effect of diabetes-specific oral nutritional supplements with allulose on weight and glycemic profiles in overweight or obese type 2 diabetic patients
Jihye Tak, Minkyung Bok, Hyunkyung Rho, Ju Hyun Park, Yunsook Lim, Suk Chon, Hyunjung Lim
Nutrition Research and Practice.2023; 17(2): 241. CrossRef - Associations Between Modifiable Risk Factors and Changes in Glycemic Status Among Individuals With Prediabetes
Salma Nabila, Ji-Eun Kim, Jaesung Choi, JooYong Park, Aesun Shin, Sang-Ah Lee, Jong-koo Lee, Daehee Kang, Ji-Yeob Choi
Diabetes Care.2023; 46(3): 535. CrossRef - Efficacy and safety of enavogliflozin, a novel SGLT2 inhibitor, in Korean people with type 2 diabetes: A 24‐week, multicentre, randomized, double‐blind, placebo‐controlled, phase III trial
Soo Heon Kwak, Kyung Ah Han, Kyung‐Soo Kim, Jae Myung Yu, EunSook Kim, Jong Chul Won, Jun Goo Kang, Choon Hee Chung, Seungjoon Oh, Sung Hee Choi, Kyu Chang Won, Sin Gon Kim, Seung Ah Cho, Bo Young Cho, Kyong Soo Park
Diabetes, Obesity and Metabolism.2023; 25(7): 1865. CrossRef - Adjusting the Use of Glucose-Lowering Agents in the Real-World Clinical Management of People with Type 2 Diabetes: A Narrative Review
Siew Pheng Chan, Lee-Ling Lim, Juliana C. N. Chan, David R. Matthews
Diabetes Therapy.2023; 14(5): 823. CrossRef - The association of perfluoroalkyl substances (PFAS) exposure and kidney function in Korean adolescents using data from Korean National Environmental Health Survey (KoNEHS) cycle 4 (2018–2020): a cross-sectional study
Jisuk Yun, Eun-Chul Jang, Soon-Chan Kwon, Young-Sun Min, Yong-Jin Lee
Annals of Occupational and Environmental Medicine.2023;[Epub] CrossRef - A Comparison of the Pharmacokinetics and Safety of Dapagliflozin Formate, an Ester Prodrug of Dapagliflozin, to Dapagliflozin Propanediol Monohydrate in Healthy Subjects
Hyun Chul Kim, Sangmi Lee, Siyoung Sung, Eunjin Kim, In-Jin Jang, Jae-Yong Chung
Drug Design, Development and Therapy.2023; Volume 17: 1203. CrossRef - Efficacy and safety of monotherapy with enavogliflozin in Korean patients with type 2 diabetes mellitus: Results of a 12‐week, multicentre, randomized, double‐blind, placebo‐controlled, phase 2 trial
Ye Seul Yang, Kyung Wan Min, Seok‐O Park, Kyung‐Soo Kim, Jae Myung Yu, Eun‐Gyoung Hong, Sung Rae Cho, Kyu Chang Won, Yong Hyun Kim, Seungjoon Oh, Sung Hee Choi, Gwanpyo Koh, Wan Huh, Su Young Kim, Kyong Soo Park
Diabetes, Obesity and Metabolism.2023; 25(8): 2096. CrossRef - An Integrated Digital Health Care Platform for Diabetes Management With AI-Based Dietary Management: 48-Week Results From a Randomized Controlled Trial
You-Bin Lee, Gyuri Kim, Ji Eun Jun, Hyunjin Park, Woo Je Lee, You-Cheol Hwang, Jae Hyeon Kim
Diabetes Care.2023; 46(5): 959. CrossRef - Performance of Simple Fibrosis Score in Non-Alcoholic Fatty Liver Disease with and without Type 2 Diabetes
Seung Min Chung, Min Kyu Kang, Jun Sung Moon, Jung Gil Park
Endocrinology and Metabolism.2023; 38(2): 277. CrossRef - Correlation analysis of cancer incidence after pravastatin treatment
Jin Yu, Raeun Kim, Jiwon Shinn, Man Young Park, Hun-Sung Kim
Cardiovascular Prevention and Pharmacotherapy.2023; 5(2): 61. CrossRef - Comparison of the effects of gemigliptin versus glimepiride on cardiac function in patients with type 2 diabetes uncontrolled with metformin: The gemi‐heart study
Seung Min Chung, Jun Sung Moon, Jun Hwa Hong, In‐Chang Hwang, Soo Lim
Diabetes, Obesity and Metabolism.2023; 25(8): 2181. CrossRef - The era of continuous glucose monitoring and its expanded role in type 2 diabetes
Jin Yu, Jae‐Hyoung Cho, Seung‐Hwan Lee
Journal of Diabetes Investigation.2023; 14(7): 841. CrossRef - Impact of continuous glucose monitoring on glycemic control and its derived metrics in type 1 diabetes: a longitudinal study
So Hyun Cho, Seohyun Kim, You-Bin Lee, Sang-Man Jin, Kyu Yeon Hur, Gyuri Kim, Jae Hyeon Kim
Frontiers in Endocrinology.2023;[Epub] CrossRef - Impact of mental disorders on the risk of heart failure among Korean patients with diabetes: a cohort study
Tae Kyung Yoo, Kyung-Do Han, Eun-Jung Rhee, Won-Young Lee
Cardiovascular Diabetology.2023;[Epub] CrossRef - Asia-Pacific consensus recommendations for application of continuous glucose monitoring in diabetes management
Alice P.S. Kong, Soo Lim, Seung-Hyun Yoo, Linong Ji, Liming Chen, Yuqian Bao, Ester Yeoh, Siew-Pheng Chan, Chih-Yuan Wang, Viswanathan Mohan, Neale Cohen, Margaret J. McGill, Stephen M. Twigg
Diabetes Research and Clinical Practice.2023; 201: 110718. CrossRef - Chronic disease management program applied to type 2 diabetes patients and prevention of diabetic complications: a retrospective cohort study using nationwide data
Min Kyung Hyun, Jang Won Lee, Seung-Hyun Ko
BMC Public Health.2023;[Epub] CrossRef - Fatty Liver & Diabetes Statistics in Korea: Nationwide Data 2009 to 2017
Eugene Han, Kyung-Do Han, Yong-ho Lee, Kyung-Soo Kim, Sangmo Hong, Jung Hwan Park, Cheol-Young Park
Diabetes & Metabolism Journal.2023; 47(3): 347. CrossRef - Opening the Precision Diabetes Care through Digital Healthcare
Joonyub Lee, Jin Yu, Kun-Ho Yoon
Diabetes & Metabolism Journal.2023; 47(3): 307. CrossRef - Glycemia according to the Use of Continuous Glucose Monitoring among Adults with Type 1 Diabetes Mellitus in Korea: A Real-World Study
You-Bin Lee, Minjee Kim, Jae Hyeon Kim
Diabetes & Metabolism Journal.2023; 47(3): 405. CrossRef - Navigating the Seas of Glycemic Control: The Role of Continuous Glucose Monitoring in Type 1 Diabetes Mellitus
Jun Sung Moon
Diabetes & Metabolism Journal.2023; 47(3): 345. CrossRef - Lost in translation: assessing the nomenclature change for diabetic kidney disease in Japan
Tetsuya Babazono, Tatsumi Moriya
Diabetology International.2023; 14(4): 319. CrossRef - Effects of dapagliflozin compared with glimepiride on body composition in Asian patients with type 2 diabetes inadequately controlled with metformin: The BEYOND study
Hyeong Kyu Park, Kyoung‐Ah Kim, Kyung‐Wan Min, Tae‐Seo Sohn, In Kyung Jeong, Chul Woo Ahn, Nan‐Hee Kim, Ie Byung Park, Ho Chan Cho, Choon Hee Chung, Sung Hee Choi, Kang Seo Park, Seoung‐Oh Yang, Kwan Woo Lee
Diabetes, Obesity and Metabolism.2023; 25(9): 2743. CrossRef - Topic Modeling Analysis of Diabetes-Related Health Information during the Coronavirus Disease Pandemic
Soyoon Min, Jeongwon Han
Healthcare.2023; 11(13): 1871. CrossRef - Screening Test for Evaluation of Cardiovascular Disease in Patients with Diabetes
Ji-Oh Mok, Chan-Hee Jung
The Journal of Korean Diabetes.2023; 24(2): 76. CrossRef - Paradigm Shift in Management of Hyperglycemia in Patients with Type 2 Diabetes: Glucocentric versus Organ Protection
Jong Chul Won
The Journal of Korean Diabetes.2023; 24(2): 59. CrossRef - Association between type 2 diabetes mellitus and depression among Korean midlife women: a cross-sectional analysis study
You Lee Yang, Eun-Ok Im, Yunmi Kim
BMC Nursing.2023;[Epub] CrossRef - Fibrotic Burden in the Liver Differs Across Metabolic Dysfunction-Associated Fatty Liver Disease Subtypes
Tae Seop Lim, Ho Soo Chun, Soon Sun Kim, Ja Kyung Kim, Minjong Lee, Hyo Jung Cho, Seung Up Kim, Jae Youn Cheong
Gut and Liver.2023; 17(4): 610. CrossRef - Association between the number of pregnancies and cardiac target organ damages: a cross-sectional analysis of data from the Korean women’s chest pain registry (KoROSE)
Hack-Lyoung Kim, Hyun-Jin Kim, Mina Kim, Sang Min Park, Hyun Ju Yoon, Young Sup Byun, Seong-Mi Park, Mi-Seung Shin, Kyung-Soon Hong, Myung-A Kim
BMC Women's Health.2023;[Epub] CrossRef - Exercise therapy for diabetes mellitus
Chaiho Jeong, Tae-Seo Sohn
Journal of the Korean Medical Association.2023; 66(7): 427. CrossRef - Medical nutrition therapy for diabetes mellitus
Suk Chon
Journal of the Korean Medical Association.2023; 66(7): 421. CrossRef - Identification of individuals at risk of hepatocellular carcinoma: screening for clinically significant liver fibrosis in patients with T2DM
Tina Reinson, Ryan M Buchanan, Christopher D Byrne
Expert Review of Endocrinology & Metabolism.2023; 18(5): 355. CrossRef - Additive impact of diabetes and sarcopenia on all-cause and cardiovascular mortality: A longitudinal nationwide population-based study
Eyun Song, Soon Young Hwang, Min Jeong Park, Ahreum Jang, Kyeong Jin Kim, Ji Hee Yu, Nam Hoon Kim, Hye Jin Yoo, Ji A. Seo, Sin Gon Kim, Nan Hee Kim, Sei Hyun Baik, Kyung Mook Choi
Metabolism.2023; 148: 155678. CrossRef - Exposure to perfluoroalkyl and polyfluoroalkyl substances and risk of stroke in adults: a meta-analysis
Min Cheol Chang, Seung Min Chung, Sang Gyu Kwak
Reviews on Environmental Health.2023;[Epub] CrossRef - Risk of Pancreatic Cancer and Use of Dipeptidyl Peptidase 4 Inhibitors in Patients with Type 2 Diabetes: A Propensity Score-Matching Analysis
Mee Kyoung Kim, Kyungdo Han, Hyuk-Sang Kwon, Soon Jib Yoo
Endocrinology and Metabolism.2023; 38(4): 426. CrossRef - Incident infection risks depending on oral antidiabetic exposure in insulin-treated type 2 diabetes patients
Sanghwa Park, Jiseon Jeong, Yunna Woo, Yeo Jin Choi, Sooyoung Shin
Scientific Reports.2023;[Epub] CrossRef - Dyslipidemia Fact Sheet in South Korea, 2022
Eun-Sun Jin, Jee-Seon Shim, Sung Eun Kim, Jae Hyun Bae, Shinae Kang, Jong Chul Won, Min-Jeong Shin, Heung Yong Jin, Jenny Moon, Hokyou Lee, Hyeon Chang Kim, In-Kyung Jeong
Journal of Lipid and Atherosclerosis.2023; 12(3): 237. CrossRef - Diabetes Mellitus in the Elderly Adults in Korea: Based on Data from the Korea National Health and Nutrition Examination Survey 2019 to 2020
Seung-Hyun Ko, Kyung Do Han, Yong-Moon Park, Jae-Seung Yun, Kyuho Kim, Jae-Hyun Bae, Hyuk-Sang Kwon, Nan-Hee Kim
Diabetes & Metabolism Journal.2023; 47(5): 643. CrossRef - Metabolic Dysfunction-Associated Steatotic Liver Disease (MASLD): A State-of-the-Art Review
Wah-Kheong Chan, Kee-Huat Chuah, Ruveena Bhavani Rajaram, Lee-Ling Lim, Jeyakantha Ratnasingam, Shireene Ratna Vethakkan
Journal of Obesity & Metabolic Syndrome.2023; 32(3): 197. CrossRef - Management of Dyslipidemia in Patients with Diabetes Mellitus
Kyung Ae Lee
The Journal of Korean Diabetes.2023; 24(3): 111. CrossRef - 2023 Clinical Practice Guidelines for Diabetes: Management of Cardiovascular Risk Factors
Ye Seul Yang
The Journal of Korean Diabetes.2023; 24(3): 135. CrossRef - Dyslipidemia Fact Sheet in South Korea, 2022
Eun-Sun Jin, Jee-Seon Shim, Sung Eun Kim, Jae Hyun Bae, Shinae Kang, Jong Chul Won, Min-Jeong Shin, Heung Yong Jin, Jenny Moon, Hokyou Lee, Hyeon Chang Kim, In-Kyung Jeong
Diabetes & Metabolism Journal.2023; 47(5): 632. CrossRef - 2023 Clinical Practice Guidelines for Diabetes Mellitus of the Korean Diabetes Association
Jong Han Choi, Kyung Ae Lee, Joon Ho Moon, Suk Chon, Dae Jung Kim, Hyun Jin Kim, Nan Hee Kim, Ji A Seo, Mee Kyoung Kim, Jeong Hyun Lim, YoonJu Song, Ye Seul Yang, Jae Hyeon Kim, You-Bin Lee, Junghyun Noh, Kyu Yeon Hur, Jong Suk Park, Sang Youl Rhee, Hae J
Diabetes & Metabolism Journal.2023; 47(5): 575. CrossRef - Riesgo residual. Conclusiones
Ángel Cequier, José Luis Zamorano
Revista Española de Cardiología Suplementos.2023; 23: 25. CrossRef - Intake of Fruit and Glycemic Control in Korean Patients with Diabetes Mellitus Using the Korea National Health and Nutrition Examination Survey
Eunju Yoon, Ji Cheol Bae, Sunghwan Suh
Endocrinology and Metabolism.2023; 38(5): 538. CrossRef - 2023 Clinical Practice Guidelines for Diabetes
Min Kyong Moon
The Journal of Korean Diabetes.2023; 24(3): 120. CrossRef - Cumulative effect of impaired fasting glucose on the risk of dementia in middle-aged and elderly people: a nationwide cohort study
Jin Yu, Kyu-Na Lee, Hun-Sung Kim, Kyungdo Han, Seung-Hwan Lee
Scientific Reports.2023;[Epub] CrossRef - Coleus forskohlii Root Extract (ForcslimTM) as a Prospective Antidiabetic Agent: In vitro Glucose Uptake Stimulation and α-Amylase Inhibitory Effects
Firoz Hirehal Hussain Mi, Channangihalli Thimmegowda Sadashiva, Neethumol Benny, Sreedrisya Ayippakkari Kuttiattu, Ravi Subban
International Journal of Pharmacology.2023; 19(5): 730. CrossRef - Comparison of on-Statin Lipid and Lipoprotein Levels for the Prediction of First Cardiovascular Event in Type 2 Diabetes Mellitus
Ji Yoon Kim, Jimi Choi, Sin Gon Kim, Nam Hoon Kim
Diabetes & Metabolism Journal.2023; 47(6): 837. CrossRef - Differential Impact of Obesity on the Risk of Diabetes Development in Two Age Groups: Analysis from the National Health Screening Program
Tae Kyung Yoo, Kyung-Do Han, Yang-Hyun Kim, Ga Eun Nam, Sang Hyun Park, Eun-Jung Rhee, Won-Young Lee
Diabetes & Metabolism Journal.2023; 47(6): 846. CrossRef - Strategies to Maintain the Remission of Diabetes Following Metabolic Surgery
Mi Kyung Kim, Hye Soon Kim
Journal of Metabolic and Bariatric Surgery.2023; 12(2): 26. CrossRef - East Asian perspectives in metabolic and bariatric surgery
Tae Jung Oh, Hyuk‐Joon Lee, Young Min Cho
Journal of Diabetes Investigation.2022; 13(5): 756. CrossRef - Recent Updates to Clinical Practice Guidelines for Diabetes Mellitus
Jin Yu, Seung-Hwan Lee, Mee Kyoung Kim
Endocrinology and Metabolism.2022; 37(1): 26. CrossRef - Association between Physical Exercise and Glycated Hemoglobin Levels in Korean Patients Diagnosed with Diabetes
Il Yun, Hye Jin Joo, Yu Shin Park, Eun-Cheol Park
International Journal of Environmental Research and Public Health.2022; 19(6): 3280. CrossRef - Effectiveness and safety of teneligliptin added to patients with type 2 diabetes inadequately controlled by oral triple combination therapy: A multicentre, randomized, double‐blind, and placebo‐controlled study
Minyoung Lee, Woo‐je Lee, Jae Hyeon Kim, Byung‐Wan Lee
Diabetes, Obesity and Metabolism.2022; 24(6): 1105. CrossRef - Trends of severe hypoglycemia in patients with type 2 diabetes in Korea: A longitudinal nationwide cohort study
Jae‐Seung Yun, Kyungdo Han, Seung‐Hyun Ko
Journal of Diabetes Investigation.2022; 13(8): 1438. CrossRef - GLP-1 receptor agonists in diabetic kidney disease: current evidence and future directions
Ji Hee Yu, So Young Park, Da Young Lee, Nan Hee Kim, Ji A Seo
Kidney Research and Clinical Practice.2022; 41(2): 136. CrossRef - Cardiorenal Risk Profiles Among Data-Driven Type 2 Diabetes Sub-Phenotypes: A Post-Hoc Analysis of the China Health and Nutrition Survey
Hui Gao, Kan Wang, Wensui Zhao, Jianlin Zhuang, Yu Jiang, Lei Zhang, Qingping Liu, Fariba Ahmadizar
Frontiers in Endocrinology.2022;[Epub] CrossRef - Individualized Medical Nutrition Therapy for Diabetic Patients according to Diabetes Medication
Juyeon Park
The Journal of Korean Diabetes.2022; 23(1): 50. CrossRef - Critical shear stress of red blood cells as a novel integrated biomarker for screening chronic kidney diseases in cases of type 2 diabetes
Il Rae Park, Jimi Choi, Eun Young Ha, Seung Min Chung, Jun Sung Moon, Sehyun Shin, Sin Gon Kim, Kyu Chang Won
Clinical Hemorheology and Microcirculation.2022; 81(4): 293. CrossRef - Effects of exercise on reducing diabetes risk in Korean women according to menopausal status
Jung-Hwan Cho, Hye-Mi Kwon, Se-Eun Park, Ju-Hwan Yoo, Kyung-Do Han, Eun-Jung Rhee, Won-Young Lee
Cardiovascular Prevention and Pharmacotherapy.2022; 4(2): 75. CrossRef - Novel Glycemic Index Based on Continuous Glucose Monitoring to Predict Poor Clinical Outcomes in Critically Ill Patients: A Pilot Study
Eun Yeong Ha, Seung Min Chung, Il Rae Park, Yin Young Lee, Eun Young Choi, Jun Sung Moon
Frontiers in Endocrinology.2022;[Epub] CrossRef - Free Versus Fixed-Ratio Combination of Basal Insulin and GLP-1 Receptor Agonists in Type 2 Diabetes Uncontrolled With GLP-1 Receptor Agonists: A Systematic Review and Indirect Treatment Comparison
Han Na Jung, Yun Kyung Cho, Se Hee Min, Hwi Seung Kim, Ye-Jee Kim, Joong-Yeol Park, Woo Je Lee, Chang Hee Jung
Frontiers in Endocrinology.2022;[Epub] CrossRef - Obesity, hypertension, diabetes mellitus, and hypercholesterolemia in Korean adults before and during the COVID-19 pandemic: a special report of the 2020 Korea National Health and Nutrition Examination Survey
Ga Bin Lee, Yoonjung Kim, Suyeon Park, Hyeon Chang Kim, Kyungwon Oh
Epidemiology and Health.2022; 44: e2022041. CrossRef - Adherence to healthy lifestyle behaviors as a preventable risk factor for severe hypoglycemia in people with type 2 diabetes: A longitudinal nationwide cohort study
Jae‐Seung Yun, Kyungdo Han, Yong‐Moon Park, Eugene Han, Yong‐ho Lee, Seung‐Hyun Ko
Journal of Diabetes Investigation.2022; 13(9): 1533. CrossRef - Diabetes Fact Sheet in Korea 2021
Jae Hyun Bae, Kyung-Do Han, Seung-Hyun Ko, Ye Seul Yang, Jong Han Choi, Kyung Mook Choi, Hyuk-Sang Kwon, Kyu Chang Won
Diabetes & Metabolism Journal.2022; 46(3): 417. CrossRef - Comprehensive Understanding for Application in Korean Patients with Type 2 Diabetes Mellitus of the Consensus Statement on Carbohydrate-Restricted Diets by Korean Diabetes Association, Korean Society for the Study of Obesity, and Korean Society of Hyperte
Jong Han Choi, Jee-Hyun Kang, Suk Chon
Diabetes & Metabolism Journal.2022; 46(3): 377. CrossRef - Effect of Carbohydrate-Restricted Diets and Intermittent Fasting on Obesity, Type 2 Diabetes Mellitus, and Hypertension Management: Consensus Statement of the Korean Society for the Study of Obesity, Korean Diabetes Association, and Korean Society of Hype
Jong Han Choi, Yoon Jeong Cho, Hyun-Jin Kim, Seung-Hyun Ko, Suk Chon, Jee-Hyun Kang, Kyoung-Kon Kim, Eun Mi Kim, Hyun Jung Kim, Kee-Ho Song, Ga Eun Nam, Kwang Il Kim
Diabetes & Metabolism Journal.2022; 46(3): 355. CrossRef - Effect of carbohydrate-restricted diets and intermittent fasting on obesity, type 2 diabetes mellitus, and hypertension management: consensus statement of the Korean Society for the Study of obesity, Korean Diabetes Association, and Korean Society of Hype
Jong Han Choi, Yoon Jeong Cho, Hyun-Jin Kim, Seung-Hyun Ko, Suk Chon, Jee-Hyun Kang, Kyoung-Kon Kim, Eun Mi Kim, Hyun Jung Kim, Kee-Ho Song, Ga Eun Nam, Kwang Il Kim
Clinical Hypertension.2022;[Epub] CrossRef - Efficacy of Personalized Diabetes Self-care Using an Electronic Medical Record–Integrated Mobile App in Patients With Type 2 Diabetes: 6-Month Randomized Controlled Trial
Eun Young Lee, Seon-Ah Cha, Jae-Seung Yun, Sun-Young Lim, Jin-Hee Lee, Yu-Bae Ahn, Kun-Ho Yoon, Min Kyung Hyun, Seung-Hyun Ko
Journal of Medical Internet Research.2022; 24(7): e37430. CrossRef - A double‐blind, Randomized controlled trial on glucose‐lowering EFfects and safety of adding 0.25 or 0.5 mg lobeglitazone in type 2 diabetes patients with INadequate control on metformin and dipeptidyl peptidase‐4 inhibitor therapy: REFIND study
Soree Ryang, Sang Soo Kim, Ji Cheol Bae, Ji Min Han, Su Kyoung Kwon, Young Il Kim, Il Seong Nam‐Goong, Eun Sook Kim, Mi‐kyung Kim, Chang Won Lee, Soyeon Yoo, Gwanpyo Koh, Min Jeong Kwon, Jeong Hyun Park, In Joo Kim
Diabetes, Obesity and Metabolism.2022; 24(9): 1800. CrossRef - Hypoglycemic agents and glycemic variability in individuals with type 2 diabetes: A systematic review and network meta-analysis
SuA Oh, Sujata Purja, Hocheol Shin, Minji Kim, Eunyoung Kim
Diabetes and Vascular Disease Research.2022; 19(3): 147916412211068. CrossRef - Tolerability and Effectiveness of Switching to Dulaglutide in Patients With Type 2 Diabetes Inadequately Controlled With Insulin Therapy
Youngsook Kim, Ji Hye Huh, Minyoung Lee, Eun Seok Kang, Bong-Soo Cha, Byung-Wan Lee
Frontiers in Endocrinology.2022;[Epub] CrossRef - Factors Influencing the Utilization of Diabetes Complication Tests Under the COVID-19 Pandemic: Machine Learning Approach
Haewon Byeon
Frontiers in Endocrinology.2022;[Epub] CrossRef - Association of prediabetes with death and diabetic complications in older adults: the pros and cons of active screening for prediabetes
Giwoong Choi, Hojun Yoon, Hyun Ho Choi, Kyoung Hwa Ha, Dae Jung Kim
Age and Ageing.2022;[Epub] CrossRef - Recent information on test utilization and intraindividual change in anti-glutamic acid decarboxylase antibody in Korea: a retrospective study
Rihwa Choi, Wonseo Park, Gayoung Chun, Jiwon Lee, Sang Gon Lee, Eun Hee Lee
BMJ Open Diabetes Research & Care.2022; 10(3): e002739. CrossRef - Extra-Glycemic Effects of Anti-Diabetic Medications: Two Birds with One Stone?
Eun-Jung Rhee
Endocrinology and Metabolism.2022; 37(3): 415. CrossRef - Pharmacological Treatment of Nonalcoholic Fatty Liver Disease: Antidiabetic Agents
Kyung-Soo Kim
The Journal of Korean Diabetes.2022; 23(2): 83. CrossRef - Maintaining Physical Activity Is Associated with Reduced Major Adverse Cardiovascular Events in People Newly Diagnosed with Diabetes
Duhoe Kim, Jaehun Seo, Kyoung Hwa Ha, Dae Jung Kim
Journal of Obesity & Metabolic Syndrome.2022; 31(2): 187. CrossRef - Effect of Carbohydrate-Restricted Diets and Intermittent Fasting on Obesity, Type 2 Diabetes Mellitus, and Hypertension Management: Consensus Statement of the Korean Society for the Study of Obesity, Korean Diabetes Association, and Korean Society of Hype
Jong Han Choi, Yoon Jeong Cho, Hyun-Jin Kim, Seung-Hyun Ko, Suk Chon, Jee-Hyun Kang, Kyoung-Kon Kim, Eun Mi Kim, Hyun Jung Kim, Kee-Ho Song, Ga Eun Nam, Kwang Il Kim
Journal of Obesity & Metabolic Syndrome.2022; 31(2): 100. CrossRef - Advanced Glycation End Products and Their Effect on Vascular Complications in Type 2 Diabetes Mellitus
Jeongmin Lee, Jae-Seung Yun, Seung-Hyun Ko
Nutrients.2022; 14(15): 3086. CrossRef - Severe hypoglycemia as a risk factor for cardiovascular outcomes in patients with type 2 diabetes: is it preventable?
Seung-Hyun Ko
Cardiovascular Prevention and Pharmacotherapy.2022; 4(3): 106. CrossRef - New, Novel Lipid-Lowering Agents for Reducing Cardiovascular Risk: Beyond Statins
Kyuho Kim, Henry N. Ginsberg, Sung Hee Choi
Diabetes & Metabolism Journal.2022; 46(4): 517. CrossRef - Current status of obesity treatment in Korea: based on the 2020 Korean Society for the Study of Obesity guidelines for obesity management
Eun-Jung Rhee
Journal of the Korean Medical Association.2022; 65(7): 388. CrossRef - Experiences of Using Wearable Continuous Glucose Monitors in Adults With Diabetes: A Qualitative Descriptive Study
Hee Sun Kang, Hyang Rang Park, Chun-Ja Kim, Savitri Singh-Carlson
The Science of Diabetes Self-Management and Care.2022; 48(5): 362. CrossRef - 젊은 2형 당뇨병 환자의 관리
재현 배
Public Health Weekly Report.2022; 15(35): 2474. CrossRef - Real-World Prescription Patterns and Barriers Related to the Use of Sodium-Glucose Cotransporter 2 Inhibitors among Korean Patients with Type 2 Diabetes Mellitus and Cardiovascular Disease
Jong Ha Baek, Ye Seul Yang, Seung-Hyun Ko, Kyung Do Han, Jae Hyeon Kim, Min Kyong Moon, Jong Suk Park, Byung-Wan Lee, Tae Jung Oh, Suk Chon, Jong Han Choi, Kyu Yeon Hur
Diabetes & Metabolism Journal.2022; 46(5): 701. CrossRef - Low-Density Lipoprotein Cholesterol Level, Statin Use and Myocardial Infarction Risk in Young Adults
Heekyoung Jeong, Kyungdo Han, Soon Jib Yoo, Mee Kyoung Kim
Journal of Lipid and Atherosclerosis.2022; 11(3): 288. CrossRef - Blood Pressure Target in Type 2 Diabetes Mellitus
Hyun-Jin Kim, Kwang-il Kim
Diabetes & Metabolism Journal.2022; 46(5): 667. CrossRef - Association of underweight status with the risk of tuberculosis: a nationwide population-based cohort study
Su Hwan Cho, Hyun Lee, Hyuktae Kwon, Dong Wook Shin, Hee-Kyung Joh, Kyungdo Han, Jin Ho Park, Belong Cho
Scientific Reports.2022;[Epub] CrossRef - Exploring the risk factors of impaired fasting glucose in middle-aged population living in South Korean communities by using categorical boosting machine
Haewon Byeon
Frontiers in Endocrinology.2022;[Epub] CrossRef - External validation and clinical application of the predictive model for severe hypoglycemia
Jae-Seung Yun, Kyungdo Han, Soo-Yeon Choi, Seon-Ah Cha, Yu-Bae Ahn, Seung-Hyun Ko
Frontiers in Endocrinology.2022;[Epub] CrossRef - Effect of Euonymus alatus Extracts on Diabetes Related Markers in Pancreatic β-Cells and C57BL/Ksj-db/db Mice
Ye Rin Kim, Eun-young Kim, Seong Uk Lee, Young Wan Kim, Yoon Hee Kim
Journal of the Korean Society of Food Science and Nutrition.2022; 51(9): 894. CrossRef - Muscle fat contents rather than muscle mass determines nonalcoholic steatohepatitis and liver fibrosis in patients with severe obesity
Eugene Han, Mi Kyung Kim, Hye Won Lee, Seungwan Ryu, Hye Soon Kim, Byoung Kuk Jang, Youngsung Suh
Obesity.2022; 30(12): 2440. CrossRef - Correlation between shift work and non-alcoholic fatty liver disease among male workers in the steel manufacturing company of Korea: a cross-sectional study
Kiseok Kim, Yong-Jin Lee, Soon-Chan Kwon, Young-Sun Min, Hyun Kyo Lee, Gwangin Baek, Sang Hyeon Kim, Eun-Chul Jang
Annals of Occupational and Environmental Medicine.2022;[Epub] CrossRef - FGM-based remote intervention for adults with type 1 diabetes: The FRIEND randomized clinical trial
Jinju Lee, Myeong Hoon Lee, Jiyun Park, Kyung-Soo Kim, Soo-Kyung Kim, Yong-Wook Cho, Hyun Wook Han, Young Shin Song
Frontiers in Endocrinology.2022;[Epub] CrossRef - Screening for Prediabetes and Diabetes in Korean Nonpregnant Adults: A Position Statement of the Korean Diabetes Association, 2022
Kyung Ae Lee, Dae Jung Kim, Kyungdo Han, Suk Chon, Min Kyong Moon
Diabetes & Metabolism Journal.2022; 46(6): 819. CrossRef - Blood Pressure Control in Patients with Diabetic Kidney Disease
Yaeni Kim, Won Kim, Jwa-Kyung Kim, Ju Young Moon, Samel Park, Cheol Whee Park, Hoon Suk Park, Sang Heon Song, Tae-Hyun Yoo, So-Young Lee, Eun Young Lee, Jeonghwan Lee, Kyubok Jin, Dae Ryong Cha, Jin Joo Cha, Sang Youb Han
Electrolytes & Blood Pressure.2022; 20(2): 39. CrossRef - The Gangwon Obesity and Metabolic Syndrome Study: Methods and Initial Baseline Data
Yoon Jeong Cho, Sohyun Park, Sung Soo Kim, Hyo Jin Park, Jang Won Son, Tae Kyung Lee, Sangmo Hong, Jee-Hyun Kang, Seon Mee Kim, Yang-Hyun Kim, Won Jun Kim, Young Eun Seo, Yoosuk An, Sang Youl Rhee, Suk Chon, Sookyoung Jeon, Kyungho Park, Bong-Soo Kim, Cha
Journal of Obesity & Metabolic Syndrome.2022; 31(4): 303. CrossRef - Oral Semaglutide, the First Ingestible Glucagon-Like Peptide-1 Receptor Agonist: Could It Be a Magic Bullet for Type 2 Diabetes?
Hwi Seung Kim, Chang Hee Jung
International Journal of Molecular Sciences.2021; 22(18): 9936. CrossRef - Long-term effectiveness and safety of quadruple combination therapy with empagliflozin versus dapagliflozin in patients with type 2 diabetes: 3-year prospective observational study
Eu Jeong Ku, Dong-Hwa Lee, Hyun Jeong Jeon, Tae Keun Oh
Diabetes Research and Clinical Practice.2021; 182: 109123. CrossRef - Albuminuria Is Associated with Steatosis Burden in Patients with Type 2 Diabetes Mellitus and Nonalcoholic Fatty Liver Disease (Diabetes Metab J 2021;45:698-707)
Mi-kyung Kim
Diabetes & Metabolism Journal.2021; 45(6): 968. CrossRef - Incidence and Risk Factors for Progression to Diabetes Mellitus: A Retrospective Cohort Study
Min Kyung Hyun, Jong Heon Park, Kyoung Hoon Kim, Soon-Ki Ahn, Seon Mi Ji
International Journal of Environmental Research and Public Health.2021; 19(1): 123. CrossRef - 2021 Clinical Practice Guidelines for Diabetes: Pharmacotherapy and the Korean Diabetes Association Support System
Kyu Yeon Hur
The Journal of Korean Diabetes.2021; 22(4): 250. CrossRef - 2021 Clinical Practice Guidelines for Diabetes: Management of Cardiovascular Risk
Min Kyong Moon
The Journal of Korean Diabetes.2021; 22(4): 259. CrossRef
- Impact of Subclinical Atrial Function on the Prognosis of Patients With Atrial Fibrillation and Metabolic Syndrome
- Obesity and Metabolic Syndrome
- Association between Blood Mercury Level and Visceral Adiposity in Adults
- Jong Suk Park, Kyoung Hwa Ha, Ka He, Dae Jung Kim
- Diabetes Metab J. 2017;41(2):113-120. Published online December 21, 2016
- DOI: https://doi.org/10.4093/dmj.2017.41.2.113
- 4,876 View
- 46 Download
- 38 Web of Science
- 39 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background Few studies have examined the association between mercury exposure and obesity. The aim of this study is to investigate the association between blood mercury concentrations and indices of obesity in adults.
Methods A total of 200 healthy subjects, aged 30 to 64 years, who had no history of cardiovascular or malignant disease, were examined. Anthropometric and various biochemical profiles were measured. Visceral adipose tissue (VAT) was measured using dual-energy X-ray absorptiometry (DXA).
Results All subjects were divided into three groups according to blood mercury concentrations. Compared with the subjects in the lowest tertile of mercury, those in the highest tertile were more likely to be male; were current alcohol drinkers and smokers; had a higher body mass index (BMI), waist circumference (WC), and VAT; had higher levels of blood pressure, fasting glucose, and insulin resistance; and consumed more fish. The blood mercury concentration was significantly associated with anthropometric parameters, showing relationships with BMI, WC, and VAT. After adjusting for multiple risk factors, the odds ratios (ORs) for high mercury concentration was significantly higher in the highest VAT tertile than in the lowest VAT tertile (OR, 2.66; 95% confidence interval, 1.05 to 6.62;
P <0.05).Conclusion The blood mercury concentration was significantly associated with VAT in healthy adults. Further studies are warranted to confirm our findings.
-
Citations
Citations to this article as recorded by- Exposure to Metal Mixtures and Overweight or Obesity Among Chinese Adults
Gaojie Fan, Qing Liu, Mingyang Wu, Jianing Bi, Xiya Qin, Qing Fang, Zhengce Wan, Yongman Lv, Youjie Wang, Lulu Song
Biological Trace Element Research.2023; 201(8): 3697. CrossRef - Methylmercury drives lipid droplet formation and adipokine expression during the late stages of adipocyte differentiation in 3T3-L1 cells
Yasukazu Takanezawa, Yui Kashiwano, Ryosuke Nakamura, Yuka Ohshiro, Shimpei Uraguchi, Masako Kiyono
Toxicology.2023; 486: 153446. CrossRef - Expression Profiling of Adipogenic and Anti-Adipogenic MicroRNA Sequences following Methylmercury Exposure in Caenorhabditis elegans
Giancarlo Garofalo, Tyson Nielsen, Samuel Caito
Toxics.2023; 11(11): 934. CrossRef - Report of the Scientific Committee of the Spanish Agency for Food Safety and Nutrition (AESAN) on the available evidence in relation to the potential obesogenic activity of certain chemical compounds that may be present in foods
Ana María Rivas Velasco, Irene Bretón Lesmes, Araceli Díaz Perales, Ángel Gil Izquierdo, María José González Muñoz, Victoria Moreno Arribas, María del Puy Portillo Baquedano, Silvia Pichardo Sánchez
Food Risk Assess Europe.2023;[Epub] CrossRef - Lead, mercury, and cadmium exposures are associated with obesity but not with diabetes mellitus: Korean National Environmental Health Survey (KoNEHS) 2015–2017
Min Kyong Moon, Inae Lee, Aram Lee, Hyunwoong Park, Min Joo Kim, Sunmi Kim, Yoon Hee Cho, Sooyeon Hong, Jiyoung Yoo, Gi Jeong Cheon, Kyungho Choi, Young Joo Park, Jeongim Park
Environmental Research.2022; 204: 111888. CrossRef - The Effect of Mixture of Heavy Metals on Obesity in Individuals ≥50 Years of Age
Hai Nguyen Duc, Hojin Oh, Min-Sun Kim
Biological Trace Element Research.2022; 200(8): 3554. CrossRef - MicroRNA Expression Influences Methylmercury-Induced Lipid Accumulation and Mitochondrial Toxicity in Caenorhabditis elegans
Tyson Nielsen, Nicole Crawford, Megan Martell, Belal Khalil, Farooq Imtiaz, Jennifer L. Newell-Caito, Samuel Caito
Chemical Research in Toxicology.2022; 35(1): 77. CrossRef - Relationship Between Serum Levels of Arsenic, Cadmium, and Mercury and Body Mass Index and Fasting Plasma Glucose in a Mexican Adult Population
Héctor Hernández-Mendoza, Héctor Edmundo Álvarez-Loredo, Elizabeth Teresita Romero-Guzmán, Darío Gaytán-Hernández, Consuelo Chang-Rueda, Israel Martínez-Navarro, Bertha Irene Juárez-Flores, María Judith Rios-Lugo
Biological Trace Element Research.2022; 200(12): 4916. CrossRef - Heavy metal-induced lipogenic gene aberration, lipid dysregulation and obesogenic effect: a review
Yang Zhou, Frank Peprah Addai, Xinshuang Zhang, Yuelin Liu, Yinfeng Wang, Feng Lin, Alex Tuffour, Jie Gu, Guangxiang Liu, Haifeng Shi
Environmental Chemistry Letters.2022; 20(3): 1611. CrossRef - Differential fat accumulation in early adulthood according to adolescent‐BMI and heavy metal exposure
Larissa Betanzos‐Robledo, Martha M. Téllez‐Rojo, Hector Lamadrid‐Figueroa, Ernesto Roldan‐Valadez, Karen E. Peterson, Erica C. Jansen, Nil Basu, Alejandra Cantoral
New Directions for Child and Adolescent Development.2022; 2022(181-182): 37. CrossRef - The Association of Mercury and ALT with Obesity in Korean Adults: Using Data from the Korea National Health and Nutrition Examination Survey for 11 Years (KNHANES 2005, 2008~2017)
Sang Shin Pyo
Korean Journal of Clinical Laboratory Science.2022; 54(3): 192. CrossRef - Plasma titanium level is positively associated with metabolic syndrome: A survey in China’s heavy metal polluted regions
Miao Huang, Jingyuan Chen, Guangyu Yan, Yiping Yang, Dan Luo, Xiang Chen, Meian He, Hong Yuan, Zhijun Huang, Yao Lu
Ecotoxicology and Environmental Safety.2021; 208: 111435. CrossRef - Relationship Between Elevated Hair Mercury Levels, Essential Element Status, and Metabolic Profile in Overweight and Obese Adults
Anatoly V. Skalny, Jung-Su Chang, Igor P. Bobrovnitsky, Philippe Yu Kopylov, Margarita G. Skalnaya, Shih-Yi Huang, Monica Maria Bastos Paoliello, Ekaterina S. Ivanova, Weu Wang, Alexey A. Tinkov
Biological Trace Element Research.2021; 199(8): 2874. CrossRef - Associations between metabolic syndrome and four heavy metals: A systematic review and meta-analysis
Ping Xu, Aiping Liu, Fengna Li, Alexey A. Tinkov, Longjian Liu, Ji-Chang Zhou
Environmental Pollution.2021; 273: 116480. CrossRef - Cadmium, lead and mercury in the blood of psoriatic and vitiligo patients and their possible associations with dietary habits
Marta Wacewicz-Muczyńska, Katarzyna Socha, Jolanta Soroczyńska, Marek Niczyporuk, Maria H. Borawska
Science of The Total Environment.2021; 757: 143967. CrossRef - Crude oil and public health issues in Niger Delta, Nigeria: Much ado about the inevitable
Orish Ebere Orisakwe
Environmental Research.2021; 194: 110725. CrossRef - Mercury in the human adrenal medulla could contribute to increased plasma noradrenaline in aging
Roger Pamphlett, Stephen Kum Jew, Philip A. Doble, David P. Bishop
Scientific Reports.2021;[Epub] CrossRef - Multiple metal exposure and obesity: A prospective cohort study of adults living along the Yangtze River, China
Qi Zhong, Qi-rong Qin, Wan-jun Yang, Jia-liu He, Jin-liang Zhu, Zhen-yu Zhu, Fen Huang
Environmental Pollution.2021; 285: 117150. CrossRef - Association between Blood Mercury Levels and Non-Alcoholic Fatty Liver Disease in Non-Obese Populations: The Korean National Environmental Health Survey (KoNEHS) 2012–2014
Yun-Jung Yang, Eun-Jung Yang, Kyongjin Park, Subin Oh, Taehyen Kim, Yeon-Pyo Hong
International Journal of Environmental Research and Public Health.2021; 18(12): 6412. CrossRef - Hair Lead, Aluminum, and Other Toxic Metals in Normal-Weight and Obese Patients with Coronary Heart Disease
Anatoly V. Skalny, Philippe Yu Kopylov, Monica M. B. Paoliello, Jung-Su Chang, Michael Aschner, Igor P. Bobrovnitsky, Jane C.-J. Chao, Jan Aaseth, Sergei N. Chebotarev, Alexey A. Tinkov
International Journal of Environmental Research and Public Health.2021; 18(15): 8195. CrossRef - Methylmercury chronic exposure affects the expression of DNA single-strand break repair genes, induces oxidative stress, and chromosomal abnormalities in young dyslipidemic APOE knockout mice
Cássia R. Roque, Letícia R. Sampaio, Mayumi N. Ito, Daniel V. Pinto, Juan S.R. Caminha, Paulo I.G. Nunes, Ramon S. Raposo, Flávia A. Santos, Cláudia C. Windmöller, Maria Elena Crespo-Lopez, Jacqueline I. Alvarez-Leite, Reinaldo B. Oriá, Ronald F. Pinheiro
Toxicology.2021; 464: 152992. CrossRef - Methylmercury-Induced Metabolic Alterations in Caenorhabditis elegans Are Diet-Dependent
Nicole Crawford, Megan Martell, Tyson Nielsen, Belal Khalil, Farooq Imtiaz, Etienne Nguidjo, Jennifer Newell-Caito, Julia Bornhorst, Tanja Schwerdtle, Samuel Caito
Toxics.2021; 9(11): 287. CrossRef - Antioxidant status in relation to heavy metals induced oxidative stress in patients with polycystic ovarian syndrome (PCOS)
Manal Abudawood, Hajera Tabassum, Atheer H. Alanazi, Fatmah Almusallam, Feda Aljaser, Mir Naiman Ali, Naif D. Alenzi, Samyah T. Alanazi, Manal A. Alghamdi, Ghadah H. Altoum, Manar A. Alzeer, Majed O. Alotaibi, Arwa Abudawood, Hazem K. Ghneim, Lulu Abdulla
Scientific Reports.2021;[Epub] CrossRef - Association of Blood Mercury Levels with the Risks of Overweight and High Waist-to-Height Ratio in Children and Adolescents: Data from the Korean National Health and Nutrition Examination Survey
Ky Young Cho
Children.2021; 8(12): 1087. CrossRef - The sex-specific effects of blood lead, mercury, and cadmium levels on hepatic steatosis and fibrosis: Korean nationwide cross-sectional study
Seung Min Chung, Jun Sung Moon, Ji Sung Yoon, Kyu Chang Won, Hyoung Woo Lee
Journal of Trace Elements in Medicine and Biology.2020; 62: 126601. CrossRef - Elevated blood mercury level has a non-linear association with infertility in U.S. women: Data from the NHANES 2013–2016
Fangfang Zhu, Chi Chen, Yingxuan Zhang, Si Chen, Xian Huang, Jingwei Li, Yanxi Wang, Xiaorong Liu, Gaopi Deng, Jie Gao
Reproductive Toxicology.2020; 91: 53. CrossRef - Methylmercury Induces Metabolic Alterations in Caenorhabditis elegans: Role for C/EBP Transcription Factor
Samuel W Caito, Jennifer Newell-Caito, Megan Martell, Nicole Crawford, Michael Aschner
Toxicological Sciences.2020; 174(1): 112. CrossRef - Association of Fish Consumption and Mercury Exposure During Pregnancy With Metabolic Health and Inflammatory Biomarkers in Children
Nikos Stratakis, David V. Conti, Eva Borras, Eduardo Sabido, Theano Roumeliotaki, Eleni Papadopoulou, Lydiane Agier, Xavier Basagana, Mariona Bustamante, Maribel Casas, Shohreh F. Farzan, Serena Fossati, Juan R. Gonzalez, Regina Grazuleviciene, Barbara He
JAMA Network Open.2020; 3(3): e201007. CrossRef - Elemental Analysis of Aging Human Pituitary Glands Implicates Mercury as a Contributor to the Somatopause
Roger Pamphlett, Stephen Kum Jew, Philip A. Doble, David P. Bishop
Frontiers in Endocrinology.2019;[Epub] CrossRef - Mercury leads to features of polycystic ovary syndrome in rats
Eduardo Merlo, Ingridy R.G. Schereider, Maylla R. Simões, Dalton V. Vassallo, Jones B. Graceli
Toxicology Letters.2019; 312: 45. CrossRef - In utero exposure to mercury and childhood overweight or obesity: counteracting effect of maternal folate status
Guoying Wang, Jessica DiBari, Eric Bind, Andrew M. Steffens, Jhindan Mukherjee, Tami R. Bartell, David C. Bellinger, Xiumei Hong, Yuelong Ji, Mei-Cheng Wang, Marsha Wills-Karp, Tina L. Cheng, Xiaobin Wang
BMC Medicine.2019;[Epub] CrossRef - Mercury Is Taken Up Selectively by Cells Involved in Joint, Bone, and Connective Tissue Disorders
Roger Pamphlett, Stephen Kum Jew
Frontiers in Medicine.2019;[Epub] CrossRef - Cohort Profile: The Cardiovascular and Metabolic Diseases Etiology Research Center Cohort in Korea
Jee-Seon Shim, Bo Mi Song, Jung Hyun Lee, Seung Won Lee, Ji Hye Park, Dong Phil Choi, Myung Ha Lee, Kyoung Hwa Ha, Dae Jung Kim, Sungha Park, Won-Woo Lee, Yoosik Youm, Eui-Cheol Shin, Hyeon Chang Kim
Yonsei Medical Journal.2019; 60(8): 804. CrossRef - Chronic mercury at low doses impairs white adipose tissue plasticity
Danize Aparecida Rizzetti, Patricia Corrales, Janaina Trindade Piagette, José Antonio Uranga-Ocio, Gema Medina-Gomez, Franck Maciel Peçanha, Dalton Valentim Vassallo, Marta Miguel, Giulia Alessandra Wiggers
Toxicology.2019; 418: 41. CrossRef - Associations of cumulative exposure to heavy metal mixtures with obesity and its comorbidities among U.S. adults in NHANES 2003–2014
Xin Wang, Bhramar Mukherjee, Sung Kyun Park
Environment International.2018; 121: 683. CrossRef - Blood mercury concentration in relation to metabolic and weight phenotypes using the KNHANES 2011–2013 data
Kayoung Lee
International Archives of Occupational and Environmental Health.2018; 91(2): 185. CrossRef - The association of total blood mercury levels and overweight among Korean adolescents: analysis of the Korean National Health and Nutrition Examination Survey (KNHANES) 2010–2013
Yi-Yeon Shin, In-Kyung Ryu, Mi-Jung Park, Shin-Hye Kim
Korean Journal of Pediatrics.2018; 61(4): 121. CrossRef - Heavy Metal Exposure and Metabolic Syndrome: Evidence from Human and Model System Studies
Antonio Planchart, Adrian Green, Cathrine Hoyo, Carolyn J. Mattingly
Current Environmental Health Reports.2018; 5(1): 110. CrossRef - Association between Blood Mercury Level and Visceral Adiposity in Adults
Seong-Su Moon
Diabetes & Metabolism Journal.2017; 41(2): 96. CrossRef
- Exposure to Metal Mixtures and Overweight or Obesity Among Chinese Adults
- Serum Adiponectin and Type 2 Diabetes: A 6-Year Follow-Up Cohort Study
- Sun Ha Jee, Chul Woo Ahn, Jong Suk Park, Chang Gyu Park, Hyon-Suk Kim, Sang-Hak Lee, Sungha Park, Myoungsook Lee, Chang Beom Lee, Hye Soon Park, Heejin Kimm, Sung Hee Choi, Jidong Sung, Seungjoon Oh, Hyojee Joung, Sung Rae Kim, Ho-Joong Youn, Sun Mi Kim, Hong Soo Lee, Yejin Mok, Eunmi Choi, Young Duk Yun, Soo-Jin Baek, Jaeseong Jo, Kap Bum Huh
- Diabetes Metab J. 2013;37(4):252-261. Published online August 14, 2013
- DOI: https://doi.org/10.4093/dmj.2013.37.4.252
- 5,153 View
- 40 Download
- 9 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background Studies on factors which may predict the risk of diabetes are scarce. This prospective cohort study was conducted to determine the association between adiponectin and type 2 diabetes among Korean men and women.
Methods A total of 42,845 participants who visited one of seven health examination centers located in Seoul and Gyeonggi province, Republic of Korea between 2004 and 2008 were included in this study. The incidence rates of diabetes were determined through December 2011. To evaluate the effects of adiponectin on type 2 diabetes, the Cox proportional hazard model was used.
Results Of the 40,005 participants, 959 developed type 2 diabetes during a 6-year follow-up. After the adjustment for age, body mass index (BMI), and waist circumference, the risks for type 2 diabetes in participants with normoglycemia had a 1.70-fold (95% confidence interval [CI], 1.21 to 2.38) increase in men and a 1.83-fold (95% CI, 1.17 to 2.86) increase in women with the lowest tertile of adiponectin when compared to the highest tertile of adiponectin. For participants with impaired fasting glucose (IFG), the risk for type 2 diabetes had a 1.46-fold (95% CI, 1.17 to 1.83) increase in men and a 2.52-fold (95% CI, 1.57 to 4.06) increase in women with the lowest tertile of adiponectin. Except for female participants with normoglycemia, all the risks remained significant after the adjustment for fasting glucose and other confounding variables. Surprisingly, BMI and waist circumference were not predictors of type 2 diabetes in men or women with IFG after adjustment for fasting glucose and other confounders.
Conclusion A strong association between adiponectin and diabetes was observed. The use of adiponectin as a predictor of type 2 diabetes is considered to be useful.
-
Citations
Citations to this article as recorded by- Adiponectin and metabolic cardiovascular diseases: Therapeutic opportunities and challenges
Xiaotian Lei, Sheng Qiu, Gangyi Yang, Qinan Wu
Genes & Diseases.2023; 10(4): 1525. CrossRef - Low levels of total and high-molecular-weight adiponectin may predict non-alcoholic fatty liver in Korean adults
Young-Sang Kim, Soo-Hyun Lee, Seung Geon Park, Bo Youn Won, Hyejin Chun, Doo-Yeoun Cho, Moon-Jong Kim, Ji Eun Lee, Ji-Hee Haam, Kunhee Han
Metabolism.2020; 103: 154026. CrossRef - Anti-inflammatory effects of sucrose-derived oligosaccharides produced by a constitutive mutant L. mesenteroides B-512FMCM dextransucrase in high fat diet-fed mice
Min-Gyung Kang, Hee Jae Lee, Jae-Young Cho, Kanghwa Kim, Soo Jin Yang, Doman Kim
Biochemical and Biophysical Research Communications.2016; 477(3): 350. CrossRef - Adiponectin as a Protective Factor Against the Progression Toward Type 2 Diabetes Mellitus in Postmenopausal Women
Hossein Darabi, Alireza Raeisi, Mohammad Reza Kalantarhormozi, Afshin Ostovar, Majid Assadi, Kamyar Asadipooya, Katayoun Vahdat, Sina Dobaradaran, Iraj Nabipour
Medicine.2015; 94(33): e1347. CrossRef - Effect of ketotifen in obese patients with type 2 diabetes mellitus
Sahar M. El-Haggar, Wael F. Farrag, Fedaa A. Kotkata
Journal of Diabetes and its Complications.2015; 29(3): 427. CrossRef - Smoking and Diabetes: Is the Association Mediated by Adiponectin, Leptin, or C-reactive Protein?
Esayas Haregot Hilawe, Hiroshi Yatsuya, Yuanying Li, Mayu Uemura, Chaochen Wang, Chifa Chiang, Hideaki Toyoshima, Koji Tamakoshi, Yan Zhang, Nobuo Kawazoe, Atsuko Aoyama
Journal of Epidemiology.2015; 25(2): 99. CrossRef - Association between the level of circulating adiponectin and prediabetes: A meta‐analysis
Huasheng Lai, Nie Lin, Zhenzhen Xing, Huanhuan Weng, Hua Zhang
Journal of Diabetes Investigation.2015; 6(4): 416. CrossRef - Adiponectin as a Biomarker of Osteoporosis in Postmenopausal Women: Controversies
Anna Lubkowska, Aleksandra Dobek, Jan Mieszkowski, Wojciech Garczynski, Dariusz Chlubek
Disease Markers.2014; 2014: 1. CrossRef - Modulation of adiponectin as a potential therapeutic strategy
Soo Lim, Michael J. Quon, Kwang Kon Koh
Atherosclerosis.2014; 233(2): 721. CrossRef
- Adiponectin and metabolic cardiovascular diseases: Therapeutic opportunities and challenges
- Serum Cystatin C Reflects the Progress of Albuminuria
- Jeong Seon Yoo, Young Mi Lee, Eun Hae Lee, Ji Woon Kim, Shin Young Lee, Ki-Cheon Jeong, Shin Ae Kang, Jong Suk Park, Joo Young Nam, Chul Woo Ahn, Young Duk Song, Kyung Rae Kim
- Diabetes Metab J. 2011;35(6):602-609. Published online December 26, 2011
- DOI: https://doi.org/10.4093/dmj.2011.35.6.602
- 4,550 View
- 38 Download
- 5 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background Research on the relationship between urinary albumin excretion and serum cystatin C in diabetes is restricted to cross-sectional studies. In this study, we investigated how well serial measurements of serum cystatin C level reflect changes in the urinary albumin excretion rate.
Methods We enrolled and retrospectively collected data on 1,058 participants with type 2 diabetes who were older than 18 years and who had more than 3 years of follow-up with serial measurements of albuminuria and serum cystatin C at an outpatient clinic.
Results With the use of a linear mixed model, we found that the albuminuria level for each patient over time corresponded with the annual change in serum cystatin C-based estimated glomerular filtration rate (cysC-eGFR) but did not correspond with the creatinine-based eGFR calculated by the modification of diet in renal disease formula (MDRD-eGFR). The discrepancy in the direction of the trend was smaller with cysC-eGFR than with MDRD-eGFR.
Conclusion Serum cystatin C level reflects the trend in albuminuria level more accurately than serum creatinine level in Korean type 2 diabetes mellitus patients.
-
Citations
Citations to this article as recorded by- Assessment of Cystatin C and Microalbumin as Biomarkers for Nephropathy in Patients with Type 2 Diabetes Mellitus
Bhuneshwar Yadav, Shashidhar K.N, Raveesha A, Muninarayana C.
Journal of Evolution of Medical and Dental Sciences.2021; 10(25): 1866. CrossRef - Albuminuria Is Associated with Steatosis Burden in Patients with Type 2 Diabetes Mellitus and Nonalcoholic Fatty Liver Disease
Eugene Han, Mi Kyung Kim, Byoung Kuk Jang, Hye Soon Kim
Diabetes & Metabolism Journal.2021; 45(5): 698. CrossRef - Increase of BACE1, Brain-Renal Risk Factor, Contributes to Kidney Damage in an Alzheimer’s Disease Mouse Model
Yan Shi, Feng Gao, Xiaoli Yang, Dongwei Liu, Qiuxia Han, Zhangsuo Liu, Hanyu Zhu, Yong Shen
Journal of Alzheimer's Disease.2020; 76(1): 237. CrossRef - Lower Leg Fat Depots Are Associated with Albuminuria Independently of Obesity, Insulin Resistance, and Metabolic Syndrome (Korea National Health and Nutrition Examination Surveys 2008 to 2011)
Eugene Han, Nan Hee Cho, Mi Kyung Kim, Hye Soon Kim
Diabetes & Metabolism Journal.2019; 43(4): 461. CrossRef - Evaluation of creatinine-based and cystatin C-based equations for estimation of glomerular filtration rate in type 1 diabetic patients
Caroline Pereira Domingueti, Rodrigo Bastos Fóscolo, Ana Cristina Simões e Silva, Luci Maria S. Dusse, Janice Sepúlveda Reis, Maria das Graças Carvalho, Ana Paula Fernandes, Karina Braga Gomes
Archives of Endocrinology and Metabolism.2016; 60(2): 108. CrossRef
- Assessment of Cystatin C and Microalbumin as Biomarkers for Nephropathy in Patients with Type 2 Diabetes Mellitus
- Dietary Oleate Has Beneficial Effects on Every Step of Non-Alcoholic Fatty Liver Disease Progression in a Methionine- and Choline-Deficient Diet-Fed Animal Model
- Ji Young Lee, Jae Hoon Moon, Jong Suk Park, Byung-Wan Lee, Eun Seok Kang, Chul Woo Ahn, Hyun Chul Lee, Bong Soo Cha
- Diabetes Metab J. 2011;35(5):489-496. Published online October 31, 2011
- DOI: https://doi.org/10.4093/dmj.2011.35.5.489
- 30,224 View
- 34 Download
- 17 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background Non-alcoholic fatty liver disease (NAFLD) is increasingly recognized as a major cause of liver-related morbidity and mortality. The underlying mechanisms of disease progression remain poorly understood, and primary therapy of NAFLD is not yet established. We investigated the effects of dietary oleate on the development and progression of NAFLD in a methionine- and choline-deficient (MCD) diet-fed animal model.
Methods A total of 30 C57BL/6J mice were randomly divided into three groups (
n =10 in each group) and fed various experimental diets for four weeks: chow, MCD diet, or OMCD (MCD diet with oleate, 0.5 mg/g/day). Liver samples were examined for steatohepatitis and fibrosis parameters and associated genes.Results Additional dietary oleate dramatically reduced MCD diet-induced hepatic steatosis. Hepatic carbohydrate responsive element-binding protein was overexpressed in MCD diet-fed mice, and dietary oleate prevented this overexpression (
P <0.001). Dietary oleate partially prevented MCD diet-induced serum level increases in aspartate aminotransferase and alanine aminotransferase (P <0.001, respectively). The mRNA expressions of hepatic monocyte chemoattractant protein 1, tumor necrosis factor-α and matrix metalloproteinase-9 were increased in MCD diet-fed mice, and this overexpression of inflammatory molecules was prevented by dietary oleate (P <0.001). Hepatic pericellular fibrosis was observed in MCD diet-fed mice, and dietary oleate prevented this fibrosis. Altogether, dietary oleate prevented MCD diet-induced hepatic steatosis, inflammation and fibrosis.Conclusion Dietary oleate has beneficial effects in every step of NAFLD development and progression and could be a nutritional option for NAFLD prevention and treatment.
-
Citations
Citations to this article as recorded by- Bidirectional association between NAFLD and gallstone disease: a systematic review and meta-analysis of observational studies
Shengying Gu, Shanshan Hu, Shuowen Wang, Chendong Qi, Chenyang Shi, Guorong Fan
Expert Review of Gastroenterology & Hepatology.2023; 17(3): 283. CrossRef - The Effect of Bioactive Aliment Compounds and Micronutrients on Non-Alcoholic Fatty Liver Disease
Camelia Munteanu, Betty Schwartz
Antioxidants.2023; 12(4): 903. CrossRef - Single‐cell transcriptomics stratifies organoid models of metabolic dysfunction‐associated steatotic liver disease
Anja Hess, Stefan D Gentile, Amel Ben Saad, Raza‐Ur Rahman, Tim Habboub, Daniel S Pratt, Alan C Mullen
The EMBO Journal.2023;[Epub] CrossRef - Histopathological Examination of the Effects of Tocilizumab and Dexamethasone on the Liver in Rats of Oleic Acid induced Acute Lung Injury
Funda TERZİ, Hüseyin Serkan EROL
Balıkesır Health Sciences Journal.2022;[Epub] CrossRef - Identifying Lipid Metabolites Influenced by Oleic Acid Administration Using High-Performance Liquid Chromatography–Mass Spectrometry-Based Lipidomics
Chao Xu, Dan Song, Askild L. Holck, Youyou Zhou, Rong Liu
ACS Omega.2020; 5(20): 11314. CrossRef - Causative and Sanative dynamicity of ChREBP in Hepato-Metabolic disorders
P. Vineeth Daniel, Prosenjit Mondal
European Journal of Cell Biology.2020; 99(8): 151128. CrossRef - PPARδ attenuates hepatic steatosis through autophagy-mediated fatty acid oxidation
Lei Tong, Long Wang, Shuangshuang Yao, Lina Jin, Jian Yang, Yifei Zhang, Guang Ning, Zhiguo Zhang
Cell Death & Disease.2019;[Epub] CrossRef - Butyrate Protects Mice Against Methionine–Choline-Deficient Diet-Induced Non-alcoholic Steatohepatitis by Improving Gut Barrier Function, Attenuating Inflammation and Reducing Endotoxin Levels
Jianzhong Ye, Longxian Lv, Wenrui Wu, Yating Li, Ding Shi, Daiqiong Fang, Feifei Guo, Huiyong Jiang, Ren Yan, Wanchun Ye, Lanjuan Li
Frontiers in Microbiology.2018;[Epub] CrossRef - Olive oil combined with Lycium barbarum polysaccharides attenuates liver apoptosis and inflammation induced by carbon tetrachloride in rats
Yun-Yun Chiang, Jane C.-J. Chao
Journal of Functional Foods.2018; 48: 329. CrossRef - Dietary oleic acid regulates hepatic lipogenesis through a liver X receptor-dependent signaling
Simon Ducheix, Alexandra Montagner, Arnaud Polizzi, Frédéric Lasserre, Marion Régnier, Alice Marmugi, Fadila Benhamed, Justine Bertrand-Michel, Laila Mselli-Lakhal, Nicolas Loiseau, Pascal G. Martin, Jean-Marc Lobaccaro, Laurent Ferrier, Catherine Postic,
PLOS ONE.2017; 12(7): e0181393. CrossRef - Is hepatic lipogenesis fundamental for NAFLD/NASH? A focus on the nuclear receptor coactivator PGC-1β
Simon Ducheix, Maria Carmela Vegliante, Gaetano Villani, Nicola Napoli, Carlo Sabbà, Antonio Moschetta
Cellular and Molecular Life Sciences.2016; 73(20): 3809. CrossRef - Metformin alleviates hepatosteatosis by restoring SIRT1-mediated autophagy induction via an AMP-activated protein kinase-independent pathway
Young Mi Song, Yong-ho Lee, Ji-Won Kim, Dong-Sik Ham, Eun-Seok Kang, Bong Soo Cha, Hyun Chul Lee, Byung-Wan Lee
Autophagy.2015; 11(1): 46. CrossRef - Adipokines and proinflammatory cytokines, the key mediators in the pathogenesis of nonalcoholic fatty liver disease
Sanja Stojsavljević
World Journal of Gastroenterology.2014; 20(48): 18070. CrossRef - Microglial Cell Activation Increases Saturated and Decreases Monounsaturated Fatty Acid Content, but Both Lipid Species are Proinflammatory
Emily B. Button, Andrew S. Mitchell, Marcia M. Domingos, Jessica H.‐J. Chung, Ryan M. Bradley, Ashkan Hashemi, Phillip M. Marvyn, Ashley C. Patterson, Ken D. Stark, Joe Quadrilatero, Robin E. Duncan
Lipids.2014; 49(4): 305. CrossRef - Modeling progressive non-alcoholic fatty liver disease in the laboratory mouse
Jesse D. Riordan, Joseph H. Nadeau
Mammalian Genome.2014; 25(9-10): 473. CrossRef - Rapid chromatographic method to decipher distinct alterations in lipid classes in NAFLD/NASH
Stephan Laggai, Yvette Simon, Theo Ranssweiler, Alexandra K Kiemer, Sonja M Kessler
World Journal of Hepatology.2013; 5(10): 558. CrossRef - Dimethyl sulfoxide reduces hepatocellular lipid accumulation through autophagy induction
Young Mi Song, Sun-Ok Song, Yong-Keun Jung, Eun-Seok Kang, Bong Soo Cha, Hyun Chul Lee, Byung-Wan Lee
Autophagy.2012; 8(7): 1085. CrossRef
- Bidirectional association between NAFLD and gallstone disease: a systematic review and meta-analysis of observational studies
- Response: Predictive Clinical Parameters for the Therapeutic Efficacy of Sitagliptin in Korean Type 2 Diabetes Mellitus (Diabetes Metab J 2011;35:159-65)
- Soon Ae Kim, Woo Ho Shim, Eun Hae Lee, Young Mi Lee, Sun Hee Beom, Eun Sook Kim, Jeong Seon Yoo, Ji Sun Nam, Min Ho Cho, Jong Suk Park, Chul Woo Ahn, Kyung Rae Kim
- Diabetes Metab J. 2011;35(3):300-301. Published online June 30, 2011
- DOI: https://doi.org/10.4093/dmj.2011.35.3.300
- 3,429 View
- 27 Download
- 1 Crossref
-
 PDF
PDF PubReader
PubReader -
Citations
Citations to this article as recorded by- Efficacy and Safety of Switching from Sitagliptin to Ipragliflozin in Obese Japanese Patients with Type 2 Diabetes Mellitus: A Single-Arm Multicenter Interventional Study
Kentaro Watanabe, Susumu Yamaguchi, Yoshinori Kosakai, Tetsuya Ioji, Hisamitsu Ishihara
Clinical Drug Investigation.2023; 43(12): 927. CrossRef
- Efficacy and Safety of Switching from Sitagliptin to Ipragliflozin in Obese Japanese Patients with Type 2 Diabetes Mellitus: A Single-Arm Multicenter Interventional Study
- Predictive Clinical Parameters for the Therapeutic Efficacy of Sitagliptin in Korean Type 2 Diabetes Mellitus
- Soon Ae Kim, Woo Ho Shim, Eun Hae Lee, Young Mi Lee, Sun Hee Beom, Eun Sook Kim, Jeong Seon Yoo, Ji Sun Nam, Min Ho Cho, Jong Suk Park, Chul Woo Ahn, Kyung Rae Kim
- Diabetes Metab J. 2011;35(2):159-165. Published online April 30, 2011
- DOI: https://doi.org/10.4093/dmj.2011.35.2.159
- 4,572 View
- 53 Download
- 40 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background Sitagliptin is a highly selective dipeptidyl peptide-4 (DPP-4) inhibitor that increases blood levels of active glucagon-like peptide (GLP)-1 and glucose-dependent insulinotrophic polypeptide (GIP), resulting in increased insulin secretion. While studies conducted in other countries have indicated the efficacy and safety of using sitagliptin to treat type 2 diabetes mellitus (T2DM), its predictors of effects to sitagliptin are not well understood. Therefore, we evaluated the predictive clinical parameters for the therapeutic benefits of sitagliptin when added to an ongoing metformin or sulfonylurea therapy in Korean T2DM subjects.
Methods We obtained data from 251 Korean T2DM subjects who had recently started taking sitagliptin as add-on therapy. Exclusion criteria included any insulin use. Changes in HbA1c (ΔHbA1c) and fasting plasma glucose (ΔFPG) were assessed by comparing baseline levels prior to sitagliptin administration to levels 12 and 24 weeks after treatment. Responders were defined as subjects who experienced decrease from baseline of >10% in ΔHbA1c or >20% in ΔFPG levels at 24 weeks.
Results We classified 81% of the subjects (204 out of 251) as responders. The responder group had a lower mean body mass index (23.70±2.40 vs. 26.00±2.26,
P ≤0.01) and were younger (58.83±11.57 years vs. 62.87±12.09 years,P =0.03) than the non-responder group.Conclusion In Korean T2DM subjects, sitagliptin responders had lower body mass index and were younger compared to non-responders.
-
Citations
Citations to this article as recorded by- Predictors of Responsiveness to GLP-1 Receptor Agonists in Insulin-Treated Patients with Type 2 Diabetes
Colleen Gavigan, Thomas Donner, Christian S. Goebl
Journal of Diabetes Research.2023; 2023: 1. CrossRef - Comparative Effects of Metformin and Dipeptidyl Peptidase-4 Inhibitors in Japanese Obese Patients with Type 2 Diabetes: A Claims Database Study
Masato Odawara, Sumiko Aoi, Tomomi Takeshima, Kosuke Iwasaki
Diabetes Therapy.2021; 12(8): 2165. CrossRef - Reduction in HbA1c with SGLT2 inhibitors vs. DPP-4 inhibitors as add-ons to metformin monotherapy according to baseline HbA1c: A systematic review of randomized controlled trials
A.J. Scheen
Diabetes & Metabolism.2020; 46(3): 186. CrossRef - Factors associated with the glucose‐lowering efficacy of sitagliptin in Japanese patients with type 2 diabetes mellitus: Pooled analysis of Japanese clinical trials
Naoko Tajima, Jun‐ichi Eiki, Taro Okamoto, Kotoba Okuyama, Masaru Kawashima, Samuel S Engel
Journal of Diabetes Investigation.2020; 11(3): 640. CrossRef - Development of a 13C Stable Isotope Assay for Dipeptidyl Peptidase-4 Enzyme Activity A New Breath Test for Dipeptidyl Peptidase Activity
Roger Yazbeck, Simone Jaenisch, Michelle Squire, Catherine A. Abbott, Emma Parkinson-Lawrence, Douglas A. Brooks, Ross N. Butler
Scientific Reports.2019;[Epub] CrossRef - Pharmacogenetics of dipeptidyl peptidase 4 inhibitors in a Taiwanese population with type 2 diabetes
Wen-Ling Liao, Wen-Jane Lee, Ching-Chu Chen, Chieh Hsiang Lu, Chien-Hsiun Chen, Yi-Chun Chou, I-Te Lee, Wayne H-H Sheu, Jer-Yuarn Wu, Chi-Fan Yang, Chung-Hsing Wang, Fuu-Jen Tsai
Oncotarget.2017; 8(11): 18050. CrossRef - Efficacy and safety of canagliflozin as add‐on therapy to teneligliptin in Japanese patients with type 2 diabetes mellitus: Results of a 24‐week, randomized, double‐blind, placebo‐controlled trial
Takashi Kadowaki, Nobuya Inagaki, Kazuoki Kondo, Kenichi Nishimura, Genki Kaneko, Nobuko Maruyama, Nobuhiro Nakanishi, Hiroaki Iijima, Yumi Watanabe, Maki Gouda
Diabetes, Obesity and Metabolism.2017; 19(6): 874. CrossRef - A Practical Review of C-Peptide Testing in Diabetes
Emma Leighton, Christopher AR Sainsbury, Gregory C. Jones
Diabetes Therapy.2017; 8(3): 475. CrossRef - Efficacy and safety of linagliptin according to patient baseline characteristics: A pooled analysis of three phase 3 trials
S. Del Prato, S. Patel, S. Crowe, M. von Eynatten
Nutrition, Metabolism and Cardiovascular Diseases.2016; 26(10): 886. CrossRef - Soluble DPP-4 up-regulates toll-like receptors and augments inflammatory reactions, which are ameliorated by vildagliptin or mannose-6-phosphate
Dong-Sung Lee, Eun-Sol Lee, Md. Morshedul Alam, Jun-Hyeog Jang, Ho-Sub Lee, Hyuncheol Oh, Youn-Chul Kim, Zahid Manzoor, Young-Sang Koh, Dae-Gil Kang, Dae Ho Lee
Metabolism.2016; 65(2): 89. CrossRef - Efficacy of hypoglycemic treatment in type 2 diabetes stratified by age or diagnosed age: a meta-analysis
Xiaoling Cai, Wenjia Yang, Yifei Chen, Xueying Gao, Lingli Zhou, Simin Zhang, Xueyao Han, Linong Ji
Expert Opinion on Pharmacotherapy.2016; 17(12): 1591. CrossRef - Baseline Body Mass Index and the Efficacy of Hypoglycemic Treatment in Type 2 Diabetes: A Meta-Analysis
Xiaoling Cai, Wenjia Yang, Xueying Gao, Lingli Zhou, Xueyao Han, Linong Ji, Francesco Giorgino
PLOS ONE.2016; 11(12): e0166625. CrossRef - Predictive Factors for the Therapeutic Response to Concomitant Treatment with DPP-4 Inhibitors in Type 2 Diabetes with Short-Term Follow-Up
Jong-Ha Baek, Bo Ra Kim, Jeong Woo Hong, Soo Kyoung Kim, Jung Hwa Jung, Jaehoon Jung, Jong Ryeal Hahm
Kosin Medical Journal.2016; 31(2): 146. CrossRef - Complementary glucagonostatic and insulinotropic effects of DPP-4 inhibitors in the glucose-lowering action in Japanese patients with type 2 diabetes
Ken-ichi Hashimoto, Yukio Horikawa, Jun Takeda
Diabetology International.2016; 7(2): 133. CrossRef - Anagliptin and sitagliptin as add‐ons to metformin for patients with type 2 diabetes: a 24‐week, multicentre, randomized, double‐blind, active‐controlled, phase III clinical trial with a 28‐week extension
S.‐M. Jin, S. W. Park, K.‐H. Yoon, K. W. Min, K.‐H. Song, K. S. Park, J.‐Y. Park, I. B. Park, C. H. Chung, S. H. Baik, S. H. Choi, H. W. Lee, I.‐K. Lee, D.‐M. Kim, M.‐K. Lee
Diabetes, Obesity and Metabolism.2015; 17(5): 511. CrossRef - Optimal Candidates for the Switch from Glimepiride to Sitagliptin to Reduce Hypoglycemia in Patients with Type 2 Diabetes Mellitus
Hyun Min Kim, Jung Soo Lim, Byung-Wan Lee, Eun-Seok Kang, Hyun Chul Lee, Bong-Soo Cha
Endocrinology and Metabolism.2015; 30(1): 84. CrossRef - C-peptide immunoreactivity index is associated with improvement of HbA1c: 2-Year follow-up of sitagliptin use in patients with type 2 diabetes
Takeshi Nishimura, Shu Meguro, Risa Sekioka, Karin Tanaka, Yoshifumi Saisho, Junichiro Irie, Masami Tanaka, Toshihide Kawai, Hiroshi Itoh
Diabetes Research and Clinical Practice.2015; 108(3): 441. CrossRef - Clinical Characteristics and Metabolic Predictors of Rapid Responders to Dipeptidyl Peptidase-4 Inhibitor as an Add-on Therapy to Sulfonylurea and Metformin
Ye An Kim, Won Sang Yoo, Eun Shil Hong, Eu Jeong Ku, Kyeong Seon Park, Soo Lim, Young Min Cho, Kyong Soo Park, Hak Chul Jang, Sung Hee Choi
Diabetes & Metabolism Journal.2015; 39(6): 489. CrossRef - Response to the dipeptidyl peptidase‐4 inhibitors in Japanese patients with type 2 diabetes might be associated with a diplotype of two single nucleotide polymorphisms on the interleukin‐6 promoter region under a certain level of physical activity
Mizue Matsui, Yoshihiko Takahashi, Noriko Takebe, Kazuma Takahashi, Kan Nagasawa, Hiroyuki Honma, Tomoyasu Oda, Mitsutaka Ono, Riyuki Nakagawa, Takayoshi Sasai, Hirobumi Togashi, Mari Hangai, Takashi Kajiwara, Haruhito Taneichi, Yasushi Ishigaki, Jo Satoh
Journal of Diabetes Investigation.2015; 6(2): 173. CrossRef - Effects of Sitagliptin on Insulin and Glucagon Levels in Type 2 Diabetes Mellitus
Ji Hyun Kim
Diabetes & Metabolism Journal.2015; 39(4): 304. CrossRef - Effects of 6-Month Sitagliptin Treatment on Insulin and Glucagon Responses in Korean Patients with Type 2 Diabetes Mellitus
Hae Kyung Yang, Borami Kang, Seung-Hwan Lee, Hun-Sung Kim, Kun-Ho Yoon, Bong-Yun Cha, Jae-Hyoung Cho
Diabetes & Metabolism Journal.2015; 39(4): 335. CrossRef - GLP-1: The Oracle for Gastric Bypass?
Gema Frühbeck, Ruben Nogueiras
Diabetes.2014; 63(2): 399. CrossRef - Effects of concomitant drugs on sitagliptin-mediated improvement in glycemic control in Japanese patients with type 2 diabetes
Takumi Hirata, Kouichi Inukai, Jiro Morimoto, Shigehiro Katayama, Hitoshi Ishida
Primary Care Diabetes.2014; 8(3): 265. CrossRef - Predictive clinical parameters for the hemoglobin A1c-lowering effect of vildagliptin in Japanese patients with type 2 diabetes
Yukihiro Bando, Masayuki Yamada, Keiko Aoki, Hideo Kanehara, Azusa Hisada, Kazuhiro Okafuji, Daisyu Toya, Nobuyoshi Tanaka
Diabetology International.2014; 5(4): 229. CrossRef - The Effect of DPP-4 Inhibitors on Metabolic Parameters in Patients with Type 2 Diabetes
Eun Yeong Choe, Yongin Cho, Younjeong Choi, Yujung Yun, Hye Jin Wang, Obin Kwon, Byung-Wan Lee, Chul Woo Ahn, Bong Soo Cha, Hyun Chul Lee, Eun Seok Kang
Diabetes & Metabolism Journal.2014; 38(3): 211. CrossRef - Very Short-Term Effects of the Dipeptidyl Peptidase-4 Inhibitor Sitagliptin on the Secretion of Insulin, Glucagon, and Incretin Hormones in Japanese Patients with Type 2 Diabetes Mellitus: Analysis of Meal Tolerance Test Data
Kazuki Murai, Tomoyuki Katsuno, Jun-ichiro Miyagawa, Toshihiro Matsuo, Fumihiro Ochi, Masaru Tokuda, Yoshiki Kusunoki, Masayuki Miuchi, Mitsuyoshi Namba
Drugs in R&D.2014; 14(4): 301. CrossRef - Variation at the DPP4 locus influences apolipoprotein B levels in South Asians and exhibits heterogeneity in Europeans related to BMI
Swneke D. Bailey, Changchun Xie, Guillaume Paré, Alexandre Montpetit, Viswanathan Mohan, Salim Yusuf, Hertzel Gerstein, James C. Engert, Sonia S. Anand
Diabetologia.2014; 57(4): 738. CrossRef - Low-dose glimepiride with sitagliptin improves glycemic control without dose-dependency in patients with type 2 diabetes inadequately controlled on high-dose glimepiride
Rieko Umayahara, Takako Yonemoto, Chika Kyou, Kae Morishita, Tatsuo Ogawa, Yoshitaka Taguchi, Tatsuhide Inoue
Endocrine Journal.2014; 61(12): 1163. CrossRef - The clinical utility of C‐peptide measurement in the care of patients with diabetes
A. G. Jones, A. T. Hattersley
Diabetic Medicine.2013; 30(7): 803. CrossRef - Predictive clinical characteristics for the efficacy of vildagliptin monotherapy in Japanese patients with type 2 diabetes mellitus: a multicenter study
Naotsuka Okayama, Kenro Imaeda, Takashi Kato, Soji Iwase, Hideomi Ohguchi, Takashi Joh, Yoshinari Hayashi, Masaya Akao, Kohei Ogawa, Mayo Hachiya, Rei Hattori, Ryosuke Kimura, Sachie Yasui, Misao Ando, Yasunari Jinno, Nobuo Takahashi, Manabu Shimizu, Nobo
Diabetology International.2013; 4(3): 179. CrossRef - Clinical Characteristics of the Responders to Dipeptidyl Peptidase-4 Inhibitors in Korean Subjects with Type 2 Diabetes
Tae Jung Oh, Hye Seung Jung, Jae Hyun Bae, Yeong Gi Kim, Kyeong Seon Park, Young Min Cho, Kyong Soo Park, Seong Yeon Kim
Journal of Korean Medical Science.2013; 28(6): 881. CrossRef - Determinants of the HbA1c-lowering effect of sitagliptin when added to ongoing insulin therapy in Japanese patients with type 2 diabetes
Yukihiro Bando, Kazuhide Ishikura, Hideo Kanehara, Keiko Aoki, Azusa Hisada, Daisyu Toya, Nobuyoshi Tanaka
Diabetology International.2013; 4(4): 251. CrossRef - The Efficacy of Vildagliptin in Korean Patients with Type 2 Diabetes
Jun Sung Moon, Kyu Chang Won
Diabetes & Metabolism Journal.2013; 37(1): 36. CrossRef - Factors Influencing Glycemic Control Response of Sitagliptin
Gun Woo Kim, Jae Hyun Kim, Mi Young Lee, Jang Yel Shin, Young Goo Shin, Eun Ho Ha, Choon Hee Chung
The Journal of Korean Diabetes.2013; 14(4): 206. CrossRef - Sitagliptin add-on to low dosage sulphonylureas: efficacy and safety of combination therapy on glycaemic control and insulin secretion capacity in type 2 diabetes
S-I. Harashima, M. Ogura, D. Tanaka, T. Fukushima, Y. Wang, T. Koizumi, M. Aono, Y. Murata, M. Seike, N. Inagaki
International Journal of Clinical Practice.2012; 66(5): 465. CrossRef - Factors predicting therapeutic efficacy of combination treatment with sitagliptin and metformin in type 2 diabetic patients: the COSMETIC study
Soo Lim, Jee Hyun An, Hayley Shin, Ah Reum Khang, Yenna Lee, Hwa Young Ahn, Ji Won Yoon, Seon Mee Kang, Sung Hee Choi, Young Min Cho, Kyong Soo Park, Hak Chul Jang
Clinical Endocrinology.2012; 77(2): 215. CrossRef - Long-term efficacy of sitagliptin for the treatment of type 2 diabetic patients in Japan
Yuji Tajiri, Munehisa Tsuruta, Tsuyoshi Ohki, Tomoko Kato, Yuko Sasaki, Kayo Tanaka, Shusuke Kono, Masayuki Tojikubo, Kentaro Yamada
Endocrine Journal.2012; 59(3): 197. CrossRef - Comparison between sitagliptin as add‐on therapy to insulin and insulin dose‐increase therapy in uncontrolled Korean type 2 diabetes: CSI study
E. S. Hong, A. R. Khang, J. W. Yoon, S. M. Kang, S. H. Choi, K. S. Park, H. C. Jang, H. Shin, G. A. Walford, S. Lim
Diabetes, Obesity and Metabolism.2012; 14(9): 795. CrossRef - Letter: Predictive Clinical Parameters for the Therapeutic Efficacy of Sitagliptin in Korean Type 2 Diabetes Mellitus (Diabetes Metab J 2011;35:159-65)
Jee-Young Oh
Diabetes & Metabolism Journal.2011; 35(3): 298. CrossRef - Candidate Dipeptidyl Peptidase-4 Inhibitors for the Treatment of Type 2 Diabetes
Yun-Mi Jang, Dong-Lim Kim
Diabetes & Metabolism Journal.2011; 35(2): 117. CrossRef
- Predictors of Responsiveness to GLP-1 Receptor Agonists in Insulin-Treated Patients with Type 2 Diabetes
- Comparison of the Efficacy of Glimepiride, Metformin, and Rosiglitazone Monotherapy in Korean Drug-Naïve Type 2 Diabetic Patients: The Practical Evidence of Antidiabetic Monotherapy Study
- Kun Ho Yoon, Jeong Ah Shin, Hyuk Sang Kwon, Seung Hwan Lee, Kyung Wan Min, Yu Bae Ahn, Soon Jib Yoo, Kyu Jeung Ahn, Sung Woo Park, Kwan Woo Lee, Yeon Ah Sung, Tae Sun Park, Min Seon Kim, Yong Ki Kim, Moon Suk Nam, Hye Soon Kim, Ie Byung Park, Jong Suk Park, Jeong Taek Woo, Ho Young Son
- Diabetes Metab J. 2011;35(1):26-33. Published online February 28, 2011
- DOI: https://doi.org/10.4093/dmj.2011.35.1.26
- 55,963 View
- 89 Download
- 31 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background Although many anti-diabetic drugs have been used to control hyperglycemia for decades, the efficacy of commonly-used oral glucose-lowering agents in Korean type 2 diabetic patients has yet to be clearly demonstrated.
Methods We evaluated the efficacy of glimepiride, metformin, and rosiglitazone as initial treatment for drug-naïve type 2 diabetes mellitus patients in a 48-week, double-blind, randomized controlled study that included 349 Korean patients. Our primary goal was to determine the change in HbA1c levels from baseline to end point. Our secondary goal was to evaluate changes in fasting plasma glucose (FPG) levels, body weight, frequency of adverse events, and the proportion of participants achieving target HbA1c levels.
Results HbA1c levels decreased from 7.8% to 6.9% in the glimepiride group (
P <0.001), from 7.9% to 7.0% in the metformin group (P <0.001), and from 7.8% to 7.0% (P <0.001) in the rosiglitazone group. Glimepiride and rosiglitazone significantly increased body weight and metformin reduced body weight during the study period. Symptomatic hypoglycemia was more frequent in the glimepiride group and diarrhea was more frequent in the metformin group.Conclusion The efficacy of glimepiride, metformin, and rosiglitazone as antidiabetic monotherapies in drug-naïve Korean type 2 diabetic patients was similar in the three groups, with no statistical difference. This study is the first randomized controlled trial to evaluate the efficacy of commonly-used oral hypoglycemic agents in Korean type 2 diabetic patients. An additional subgroup analysis is recommended to obtain more detailed information.
-
Citations
Citations to this article as recorded by- Ketogenic Diet Intervention on Metabolic and Psychiatric Health in Bipolar and Schizophrenia: A Pilot Trial
Shebani Sethi, Diane Wakeham, Terence Ketter, Farnaz Hooshmand, Julia Bjornstad, Blair Richards, Eric Westman, Ronald M Krauss, Laura Saslow
Psychiatry Research.2024; 335: 115866. CrossRef - 2023 Clinical Practice Guidelines for Diabetes Mellitus of the Korean Diabetes Association
Jong Han Choi, Kyung Ae Lee, Joon Ho Moon, Suk Chon, Dae Jung Kim, Hyun Jin Kim, Nan Hee Kim, Ji A Seo, Mee Kyoung Kim, Jeong Hyun Lim, YoonJu Song, Ye Seul Yang, Jae Hyeon Kim, You-Bin Lee, Junghyun Noh, Kyu Yeon Hur, Jong Suk Park, Sang Youl Rhee, Hae J
Diabetes & Metabolism Journal.2023; 47(5): 575. CrossRef - The forgotten type 2 diabetes mellitus medicine: rosiglitazone
Bo Xu, Aoxiang Xing, Shuwei Li
Diabetology International.2022; 13(1): 49. CrossRef - Real-world comparison of mono and dual combination therapies of metformin, sulfonylurea, and dipeptidyl peptidase-4 inhibitors using a common data model
Kyung Ae Lee, Heung Yong Jin, Yu Ji Kim, Sang Soo Kim, Eun-Hee Cho, Tae Sun Park
Medicine.2022; 101(8): e28823. CrossRef - 2021 Clinical Practice Guidelines for Diabetes Mellitus of the Korean Diabetes Association
Kyu Yeon Hur, Min Kyong Moon, Jong Suk Park, Soo-Kyung Kim, Seung-Hwan Lee, Jae-Seung Yun, Jong Ha Baek, Junghyun Noh, Byung-Wan Lee, Tae Jung Oh, Suk Chon, Ye Seul Yang, Jang Won Son, Jong Han Choi, Kee Ho Song, Nam Hoon Kim, Sang Yong Kim, Jin Wha Kim,
Diabetes & Metabolism Journal.2021; 45(4): 461. CrossRef - A RANDOMISED, PROSPECTIVE, PARALLELAND OPEN LABEL STUDY TO COMPARE EFFICACY AND SAFETY OF METFORMIN PLUS ROSUVASTATIN AND GLIMEPIRIDE PLUS ROSUVASTATIN IN PATIENTS OF COEXISTING NON-ALCOHOLIC FATTY LIVER DISEASE (NAFLD) AND TYPE 2 DIABETES MELLITUS (T2DM)
Prabhsimran kaur, Gurpreet Kaur Randhawa, Surinder Kumar Salwan
INTERNATIONAL JOURNAL OF SCIENTIFIC RESEARCH.2021; : 46. CrossRef - Impact of sitagliptin combination therapy and hypoglycemia in Japanese patients with type 2 diabetes: a multi-center retrospective observational cohort study
Tomoyuki Saito, Hirotoshi Ohmura, Shuko Nojiri, Hiroyuki Daida
Journal of Pharmaceutical Health Care and Sciences.2020;[Epub] CrossRef - 2019 Clinical Practice Guidelines for Type 2 Diabetes Mellitus in Korea
Mee Kyoung Kim, Seung-Hyun Ko, Bo-Yeon Kim, Eun Seok Kang, Junghyun Noh, Soo-Kyung Kim, Seok-O Park, Kyu Yeon Hur, Suk Chon, Min Kyong Moon, Nan-Hee Kim, Sang Yong Kim, Sang Youl Rhee, Kang-Woo Lee, Jae Hyeon Kim, Eun-Jung Rhee, SungWan Chun, Sung Hoon Yu
Diabetes & Metabolism Journal.2019; 43(4): 398. CrossRef - Oral Hypoglycemic Agents for Patients with Type 2 Diabetes Mellitus
Seung-Hyun Ko
The Journal of Korean Diabetes.2019; 20(3): 142. CrossRef - Monotherapy in Type 2 Diabetes Mellitus Patients 2017: A Position Statement of the Korean Diabetes Association
Sang Youl Rhee
The Journal of Korean Diabetes.2018; 19(1): 15. CrossRef - Failure of monotherapy in clinical practice in patients with type 2 diabetes: The Korean National Diabetes Program
Ja Young Jeon, Soo Jin Lee, Sieun Lee, Soo Jin Kim, Seung Jin Han, Hae Jin Kim, Dae Jung Kim, Young Seol Kim, Jeong Taek Woo, Kyu Jeung Ahn, Moonsuk Nam, Sei Hyun Baik, Yongsoo Park, Kwan‐Woo Lee
Journal of Diabetes Investigation.2018; 9(5): 1144. CrossRef - Women are less likely than men to achieve optimal glycemic control after 1 year of treatment: A multi-level analysis of a Korean primary care cohort
Seung-Ah Choe, Joo Yeong Kim, Young Sun Ro, Sung-Il Cho, Antonio Palazón-Bru
PLOS ONE.2018; 13(5): e0196719. CrossRef - Monotherapy in Patients with Type 2 Diabetes Mellitus
Sang Youl Rhee, Hyun Jin Kim, Seung-Hyun Ko, Kyu-Yeon Hur, Nan-Hee Kim, Min Kyong Moon, Seok-O Park, Byung-Wan Lee, Kyung Mook Choi, Jin Hwa Kim
Diabetes & Metabolism Journal.2017; 41(5): 349. CrossRef - Antihyperglycemic Agent Therapy for Adult Patients with Type 2 Diabetes Mellitus 2017: A Position Statement of the Korean Diabetes Association
Seung-Hyun Ko, Kyu-Yeon Hur, Sang Youl Rhee, Nan-Hee Kim, Min Kyong Moon, Seok-O Park, Byung-Wan Lee, Hyun Jin Kim, Kyung Mook Choi, Jin Hwa Kim
Diabetes & Metabolism Journal.2017; 41(5): 337. CrossRef - Monotherapy in patients with type 2 diabetes mellitus
Sang Youl Rhee, Hyun Jin Kim, Seung-Hyun Ko, Kyu Yeon Hur, Nan-Hee Kim, Min Kyong Moon, Seok-O Park, Byung-Wan Lee, Kyung Mook Choi, Jin Hwa Kim
The Korean Journal of Internal Medicine.2017; 32(6): 959. CrossRef - Antihyperglycemic agent therapy for adult patients with type 2 diabetes mellitus 2017: a position statement of the Korean Diabetes Association
Seung-Hyun Ko, Kyu-Yeon Hur, Sang Youl Rhee, Nan-Hee Kim, Min Kyong Moon, Seok-O Park, Byung-Wan Lee, Hyun Jin Kim, Kyung Mook Choi, Jin Hwa Kim
The Korean Journal of Internal Medicine.2017; 32(6): 947. CrossRef - Insulin Secretory Capacity and Insulin Resistance in Korean Type 2 Diabetes Mellitus Patients
Jong-Dai Kim, Won-Young Lee
Endocrinology and Metabolism.2016; 31(3): 354. CrossRef - Trends of antidiabetic drug use in adult type 2 diabetes in Korea in 2002–2013
Seung-Hyun Ko, Dae-Jung Kim, Jong-Heon Park, Cheol-Young Park, Chang Hee Jung, Hyuk-Sang Kwon, Joong-Yeol Park, Kee-Ho Song, Kyungdo Han, Ki-Up Lee, Kyung-Soo Ko
Medicine.2016; 95(27): e4018. CrossRef - Clinical Practice Guideline 2015: Oral Hypoglycemic Agents for Patients with Type 2 Diabetes
Seung-Hyun Ko
The Journal of Korean Diabetes.2016; 17(2): 83. CrossRef - Efficacy and safety of teneligliptin, a dipeptidyl peptidase‐4 inhibitor, combined with metformin in Korean patients with type 2 diabetes mellitus: a 16‐week, randomized, double‐blind, placebo‐controlled phase III trial
M. K. Kim, E.‐J. Rhee, K. A. Han, A. C. Woo, M.‐K. Lee, B. J. Ku, C. H. Chung, K.‐A. Kim, H. W. Lee, I. B. Park, J. Y. Park, H. C. Chul Jang, K. S. Park, W. I. Jang, B. Y. Cha
Diabetes, Obesity and Metabolism.2015; 17(3): 309. CrossRef - Effect of Yanggyuksanhwa-Tang on non-insulin-dependent diabetes mellitus unresponsive to oral hypoglycemic agents: A case report
Jiman Kim, Seungwon Kwon
Chinese Journal of Integrative Medicine.2015; 21(2): 157. CrossRef - Efficacy of glimepiride/metformin fixed‐dose combination vs metformin uptitration in type 2 diabetic patients inadequately controlled on low‐dose metformin monotherapy: A randomized, open label, parallel group, multicenter study in Korea
Hye‐soon Kim, Doo‐man Kim, Bong‐soo Cha, Tae Sun Park, Kyoung‐ah Kim, Dong‐lim Kim, Choon Hee Chung, Jeong‐hyun Park, Hak Chul Jang, Dong‐seop Choi
Journal of Diabetes Investigation.2014; 5(6): 701. CrossRef - Evaluation of the Association between the Use of Oral Anti-hyperglycemic Agents and Hypoglycemia in Japan by Data Mining of the Japanese Adverse Drug Event Report (JADER) Database
Ryogo Umetsu, Yuri Nishibata, Junko Abe, Yukiya Suzuki, Hideaki Hara, Hideko Nagasawa, Yasutomi Kinosada, Mitsuhiro Nakamura
YAKUGAKU ZASSHI.2014; 134(2): 299. CrossRef - Comparative efficacy of glimepiride and metformin in monotherapy of type 2 diabetes mellitus: meta-analysis of randomized controlled trials
Hongmei Zhu, Shuang Zhu, Xiuqian Zhang, Yang Guo, Yunzhen Shi, Zhimin Chen, Siu-wai Leung
Diabetology & Metabolic Syndrome.2013;[Epub] CrossRef - A Comparative Study of the Effects of a Dipeptidyl Peptidase-IV Inhibitor and Sulfonylurea on Glucose Variability in Patients with Type 2 Diabetes with Inadequate Glycemic Control on Metformin
Hun-Sung Kim, Jeong-Ah Shin, Seung-Hwan Lee, Eun-Sook Kim, Jae-Hyoung Cho, Ho-Young Son, Kun-Ho Yoon
Diabetes Technology & Therapeutics.2013; 15(10): 810. CrossRef - Glycemic Effectiveness of Metformin-Based Dual-Combination Therapies with Sulphonylurea, Pioglitazone, or DPP4-Inhibitor in Drug-Naïve Korean Type 2 Diabetic Patients
Young Ki Lee, Sun Ok Song, Kwang Joon Kim, Yongin Cho, Younjeong Choi, Yujung Yun, Byung-Wan Lee, Eun-Seok Kang, Bong Soo Cha, Hyun Chul Lee
Diabetes & Metabolism Journal.2013; 37(6): 465. CrossRef - Metformin Based Dual-Combination Therapies in Drug Naïve Type 2 Diabetic Patients
Dong-Lim Kim
Diabetes & Metabolism Journal.2013; 37(6): 429. CrossRef - Assessing Relative Bioactivity of Chemical Substances Using Quantitative Molecular Network Topology Analysis
Anna Edberg, Daniel Soeria-Atmadja, Jonas Bergman Laurila, Fredrik Johansson, Mats G. Gustafsson, Ulf Hammerling
Journal of Chemical Information and Modeling.2012; 52(5): 1238. CrossRef - Efficacy and safety of ginsam, a vinegar extract from Panax ginseng, in type 2 diabetic patients: Results of a double‐blind, placebo‐controlled study
Ji Won Yoon, Seon Mee Kang, Jason L Vassy, Hayley Shin, Yun Hee Lee, Hwa Young Ahn, Sung Hee Choi, Kyong Soo Park, Hak Chul Jang, Soo Lim
Journal of Diabetes Investigation.2012; 3(3): 309. CrossRef - What Is the Optimal Monotherapy in Korean Drug-Naïve Type 2 Diabetic Patients?: The Practical Evidence of Antidiabetic Monotherapy Study
Ji Hun Choi, Won-Young Lee
Diabetes & Metabolism Journal.2011; 35(1): 23. CrossRef - Predictive characteristics of patients achieving glycaemic control with insulin after sulfonylurea failure
Y.-H. Lee, B.-W. Lee, S. W. Chun, B. S. Cha, H. C. Lee
International Journal of Clinical Practice.2011; 65(10): 1076. CrossRef
- Ketogenic Diet Intervention on Metabolic and Psychiatric Health in Bipolar and Schizophrenia: A Pilot Trial
- The Association of Plasma HDL-Cholesterol Level with Cardiovascular Disease Related Factors in Korean Type 2 Diabetic Patients.
- Hye Sook Hong, Jong Suk Park, Han Kyoung Ryu, Wha Young Kim
- Korean Diabetes J. 2008;32(3):215-223. Published online June 1, 2008
- DOI: https://doi.org/10.4093/kdj.2008.32.3.215
- 2,488 View
- 34 Download
- 4 Crossref
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Cardiovascular disease (CVD) is the major cause of death in type 2 diabetic patients. The purpose of this study was to investigate the characteristics of Korean type 2 diabetes mellitus (DM) patients according to plasma high density lipoprotein (HDL) cholesterol level and to document the effect of diet on HDL-cholesterol. METHODS: The subjects were 252 (male: 134, female: 118) Korean type 2 DM patients recruited from a general hospital's DM clinic and divided into low HDL-cholesterol group (male < 40 mg/dL, female < 50 mg/dL) and control group (male > or = 40 mg/dL, female > or = 50 mg/dL). Anthropometric and hematological variables and dietary intake were assessed by the groups. RESULTS: The subject's mean age was 60.2 +/- 1.1 years and duration of diabetes was 9.5 +/- 1.0 years. Anthropometric measurements (body fat mass, % body fat, WHR, fat free mass, and muscle mass) and BMI were not significantly different between two groups. The male subjects with low HDL-cholesterolemia showed higher Atherogenic Index (AI, P < 0.001) and higher % carbohydrate from energy than control group (P < 0.01). The female subjects with low HDL-cholesterolemia showed higher AI (P < 0.001) and a tendency of higher triglyceride level and lower intake of energy, protein, lipid, vitamin B1 and vitamin E (P < 0.05) than control group. CONCLUSION: The subject with low HDL-cholesterolemia showed significantly higher AI. Male subject with low HDL-cholesterolemia consumed higher carbohydrate and female subject with low HDL-cholesterolemia showed lower intakes of many nutrients. This result suggests the importance of an adequate and balanced diet to manage type 2 DM patients to prevent CVD complications. -
Citations
Citations to this article as recorded by- Improvement of High-fat Diet-induced Obesity by Xanthigen in C57BL/6N Mice
Kyeong-Mi Choi, Youn-Sun Lee, Wonkyun Kim, Yung-Hyun Choi, Youn-Gil Kwak, Jae-Chul Jung, Jeongrai Lee, Hwan-Soo Yoo
Journal of Life Science.2012; 22(12): 1697. CrossRef - The Prevalence, Awareness and Treatment of High Low Density Lipoprotein-Cholesterol in Korean Adults Without Coronary Heart Diseases - The Third Korea National Health and Nutrition Examination Survey, 2005 -
Sun-Ja Choi, Sung-Hee Park, Kwang-Soo Lee, Hyun-Young Park
Korean Circulation Journal.2012; 42(2): 86. CrossRef - Administration of Triticum aestivum Sprout Water Extracts Reduce the Level of Blood Glucose and Cholesterol in Leptin Deficient ob/ob Mice
Sun-Hee Lee, Sung-Won Lim, Nguyen Van Mihn, Jung-Mu Hur, Bong-Joon Song, Young-Mi Lee, Hoi-Seon Lee, Dae-Ki Kim
Journal of the Korean Society of Food Science and Nutrition.2011; 40(3): 401. CrossRef - Effects of Namhae Specialized Crops Water Extract on Lipid Metabolism in Rats Fed a Cholesterol Diet
Jung-Hye Shin, Min-Jung Kang, Seung-Mi Yang, Soo-Jung Lee, Nak-Ju Sung
Korean journal of food and cookery science.2011; 27(5): 599. CrossRef
- Improvement of High-fat Diet-induced Obesity by Xanthigen in C57BL/6N Mice
- In vivo Corneal Confocal Microscopy and Nerve Growth Factor in Diabetic Microvascular Complications.
- Ji Sun Nam, Young Jae Cho, Tae Woong Noh, Chul Sik Kim, Jong Suk Park, Min ho Cho, Hai Jin Kim, Ji Eun Yoon, Han Young Jung, Eun Seok Kang, Yu Mie Rhee, Hyung Keun Lee, Chul Woo Ahn, Bong Soo Cha, Eun Jig Lee, Sung Kil Lim, Kyung Rae Kim, Hyun Chul Lee
- Korean Diabetes J. 2007;31(4):351-361. Published online July 1, 2007
- DOI: https://doi.org/10.4093/jkda.2007.31.4.351
- 2,616 View
- 19 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
In vivo corneal confocal microscopy (IVCCM) is being recognized as a non-invasive, early diagnostic tool for diabetic neuropathy, for it provides a clear image of corneal subbasal nerve plexus in detail. Nerve growth factors (NGF) are believed to regulate peripheral and central nervous system, neuronal differentiation, and regeneration of damaged nerves, and their role in diabetic neuropathy is being emphasized these days. Moreover, NGFs and receptors are also expressed in retina and renal mesangial cells, suggesting their possible role in the common pathogenesis of diabetic microvascular complications. We plan to examine corneal structures of diabetic patients and compare IVCCM with conventional tools and analyze their serum and tear NGF levels. METHODS: IVCCM, nerve conduction velocity (NCV), and serum, urine, and tear samplings were done to 42 diabetic patients. From IVCCM, we measured corneal nerve density, branch, and tortuosity, total corneal/epithelial thickness, and the number of endothelial/keratocyte cells, and we checked patients' biochemical profiles and serum and tear NGF levels. RESULTS: Patients with more severe neuropathy had less corneal endothelial cells (3105 +/- 218 vs. 2537 +/- 142 vs. 2350 +/- 73/mm3 vs. 1914 +/- 465/mm3, P = 0.02), higher serum NGF (36 +/- 15 vs. 60 +/- 57.66 vs. 80 +/- 57.63 vs. 109 +/- 60.81 pg/mL, P = 0.39) and tear NGF levels (135.00 +/- 11.94 vs. 304.29 +/- 242.44 vs. 538.50 +/- 251.92 vs. 719.50 +/- 92.63 pg/mL, P = 0.01). There was a positive correlation between neuropathy and corneal nerve tortuosity (r2 = 0.479, P = 0.044) and negative correlation between neuropathy and endothelial cell count (r2 = -0.709, P = 0.002). Interestingly, similar changes were seen in other microvascular complications as well. CONCLUSION: Our results provide a possibility of using novel tools, IVCCM and NGF, as common diagnostic tools for diabetic microvascular complications, but it should be followed by a large population study.
- Activation of NF-kappaB and AP-1 in Peripheral Blood Mononuclear Cells Isolated from Patients with Diabetic Nephropathy.
- Jisun Nam, Min Ho Cho, Jong Suk Park, Geun Taek Lee, Hai Jin Kim, Eun Seok Kang, Yu Mie Lee, Chul Woo Ahn, Bong Soo Cha, Eun Jig Lee, Sung Kil Lim, Kyung Rae Kim, Hun Joo Ha, Hyun Chul Lee
- Korean Diabetes J. 2007;31(3):261-273. Published online May 1, 2007
- DOI: https://doi.org/10.4093/jkda.2007.31.3.261
- 2,083 View
- 18 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
We evaluated the role of oxidative stress in diabetic nephropathy by measuring intracellular reactive oxygen species (ROS) and redox-sensitive transcription factors in isolated peripheral mononuclear cells (PBMC). METHODS: From 66 diabetic patients with or without diabetic nephropathy (Group III and II, respectively) and 49 normal control subjects (Group I), spontaneous and stimulated ROS levels, activities of nuclear factor-kappa B (NF-kappaB), activator protein-1 (AP-1), and specificity protein1 (Sp1) in PBMC, urinary and PBMC TGF-beta1 (transforming growth factor-beta1), and 24-hour urinary albumin excretion (UAE) were measured. RESULTS: Spontaneous ROS was significantly higher in group III and II than group I (60.7 +/- 3.3 vs. 60.0 +/- 3.0 vs. 41.1 +/- 2.4%, respectively), and stimulated ROS were significantly higher in Group III compared to Group II (Increment of H2O2-induced ROS production: 21.8 +/- 2.2 vs. 11.1 +/- 2.0%, respectively; increment of PMA-induced ROS production 23.5 +/- 4.5 vs. 21.6 +/- 2.2%, respectively). The activities of NF-kappaB and AP-1, but not of Sp1, were significantly higher in Group III than in Group II (2.53 vs. 2.0 vs. 1.43-fold, respectively). Both PBMC- and urinary TGF-beta1 levels were higher in Group III than Group II (3.23 +/- 0.39 vs. 1.99 +/- 0.68 ng/mg in PBMCs, 16.88 +/- 6.84 vs. 5.61 +/- 1.57 ng/mL in urine, both respectively), and they were significantly correlated with activities of NF-kappaB and AP-1 and 24-hour UAE. CONCLUSIONS: Increased intracellular ROS generation in PBMCs of diabetic patients is involved in the pathogenesis of diabetic nephropathy through activation of NF-kappaB and AP-1, but not Sp1, and increased expression of TGF-beta1.
- Relation between Cerebral Arterial Pulsatility and Insulin Resistance in Type 2 Diabetic Patients.
- Jong Suk Park, Chul Sik Kim, Hai Jin Kim, Ji Sun Nam, Tae Woong Noh, Chul Woo Ahn, Kyung Yul Lee, Bong Soo Cha, Sung Kil Lim, Kyung Rae Kim, Hyun Chul Lee
- Korean Diabetes J. 2006;30(5):347-354. Published online September 1, 2006
- DOI: https://doi.org/10.4093/jkda.2006.30.5.347
- 2,243 View
- 18 Download
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Diabetic patients have a 3-fold risk for cerebrovascular disease compared with nondiabetic controls. The aim of the present study was to investigate the association of insulin resistance with pulsatility index (PI) of cerebral arteries in type 2 diabetic patients. METHODS: We compared a group of 90 patients with stroke free, type 2 diabetes and an age- and sex-matched control group of 45 healthy subjects without diabetes. Diabetic patients were divided into 3 groups according to the ISI (insulin sensitivity index). We evaluated PI of the middle cerebral artery (MCA) by transcranial Doppler ultrasonography (TCD) and insulin resistance determined by short insulin tolerance test. RESULTS: The PI was significantly higher in diabetic patients than that in healthy controls (P < 0.05), and also higher in patients with insulin resistance than that in insulin sensitive diabetic patients (P < 0.05). The PI of the MCA was significantly correlated with age (r= 0.465, P < 0.01), duration of diabetes (r = 0.264, P = 0.025), hypertension (r = 0.285, P = 0.015) and inversely correlated with insulin resistance (r = -0.359, P = 0.030).Multiple regression analysis was performed with PI as a dependent variable and insulin resistance as an independent variable along with known clinical risk factors. Age (beta = 0.393, P < 0.01) and duration of diabetes (beta = 0.274, P = 0.043) exhibited a significant independent contribution to PI. CONCLUSIONS: PI might be useful markers of the detection of diabetic cerebrovascular changes and insulin resistance, measured with short insulin tolerance test, showed correlations with PI, but age and duration of diabetes contributed independently to the variability in the PI. -
Citations
Citations to this article as recorded by- Factors Affecting Basilar Artery Pulsatility Index on Transcranial Doppler
Ho Tae Jeong, Dae Sik Kim, Kun Woo Kang, Yun Teak Nam, Ji Eun Oh, Eun Kyung Cho
The Korean Journal of Clinical Laboratory Science.2018; 50(4): 477. CrossRef
- Factors Affecting Basilar Artery Pulsatility Index on Transcranial Doppler
- Effects of Pioglitazone on Cerebral Hemodynamics in Patients of Type 2 Diabetes.
- Jong Suk Park, You Jung Lee, Chul Sik Kim, Hai Jin Kim, Jina Park, Chul Woo Ahn, Kyung Yul Lee, Hyeong Jin Kim, Young Jun Won, Hun Ju Ha, Hae Sun Kwak, Bong Soo Cha, Sung Kil Lim, Kyung Rae Kim, Hyun Chul Lee
- Korean Diabetes J. 2006;30(2):96-103. Published online March 1, 2006
- DOI: https://doi.org/10.4093/jkda.2006.30.2.96
- 2,644 View
- 19 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Atherosclerosis is one of the major causes of morbidity and mortality in patients with type 2 diabetes and pioglitazone has been reported to have antiatherogenic effect. The aim of this study was to investigate whether pioglitazone affects carotid intima-media thickness (IMT) and pulsatility index (PI) in type 2 diabetic patients. METHODS: A total of 40 type 2 diabetic patients were included and divided into two groups: the pioglitazone-treated group (pioglitazone 15 mg/day with gliclazide 80~320 mg/day for 12 weeks) (n = 20) and control group (gliclazide 80~320 mg/day for 12 weeks) (n = 20). The changes in lipid profile, insulin resistance, IMT, and PI were monitored to determine that pioglitazone improves cerebrovascular blood flow. RESULTS: The pioglitazone treatment significantly increased HDL-C, reduced triglyceride, insulin resistance and PI. IMT tended to decrease but the change was not significant. This study revealed that treatment with pioglitazone was associated with the improvement of cerebrovascular blood flow. CONCLUSIONS: Pioglitazone appears to be effective for the improvement of cerebrovascular blood flow in type 2 diabetic patients

 KDA
KDA
 First
First Prev
Prev





